Are those sudden flashes and jagged blind spots making you feel like you are losing control of your vision right now? We clarify the confusing ocular migraine aura by revealing the vital differences between common neurological waves and rare retinal spasms that threaten your sight while providing you with the specific tools to regain your confidence. You will master a simple physical test to pinpoint the source and learn how digital tracking tools predict these silent storms to transform your fear into a proactive plan for relief and total peace of mind.
Ocular Migraine Aura: Use the One-Eye Test for Clarity
Seeing weird shapes or flashes can be terrifying when you don’t know why. I’ve been there, staring at flickering lights and wondering if my sight was failing for good. Understanding what happens in your head starts with one simple physical gesture.
Cover One Eye to Pinpoint the Source
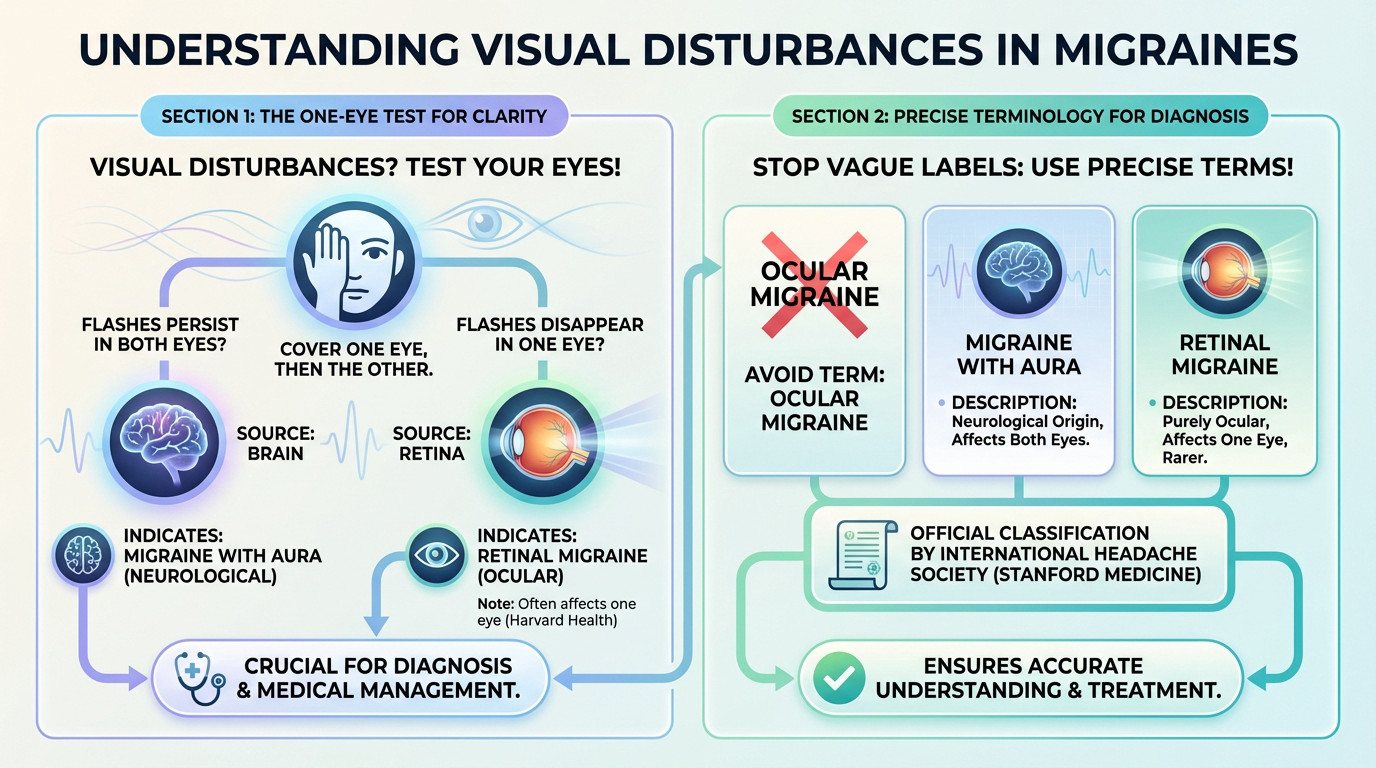
Try this right now. Close your left eye, then swap. If those flickering zigzags persist in both views, your brain is likely the culprit.
Seeing symptoms in just one eye points toward a retinal issue. This particular detail helps your doctor narrow things down.
Research from Harvard Health notes that a true ocular migraine typically strikes a single eye. It originates from the eye’s blood vessels. This distinction is vital.
Stay sharp during attacks. This tiny observation drastically shifts how we approach your long-term relief.
Stop Using Vague Labels for Clear Symptoms
We often toss around the term ocular migraine like a catch-all. Experts actually find it quite confusing. Modern specialists prefer naming these episodes as either migraine with aura or retinal migraine. Getting the name right prevents massive treatment blunders.
Specialists at Stanford Medicine follow the International Headache Society’s strict definitions. They categorize these based on where the activity starts.
Classic aura is a neurological wave. The retinal version is purely vascular, much rarer, and requires its own care.
Use precise language. It ensures your medical team understands exactly what your nervous system is doing.
References
- Harvard Health – When vision problems are actually migraine attacks
- Stanford Medicine – Stanford headache specialist demystifies migraine auras
2 Distinct Physiological Causes Behind Visual Changes
After identifying the symptoms, it’s time to look under the hood to understand why your vision is playing tricks.
Trace the Electrical Wave Across Your Brain
Cortical spreading depression is the real culprit here. It is a slow electrical wave. This silent storm travels right across your visual cortex, disrupting everything.
Closing your eyes won’t help because the brain generates these images. Your eyelids simply cannot stop those flickering zigzags.
We finally understand what is a migraine today. It is a complex, genetic neurological disease. This electrical surge is just one intense symptom.
It’s honestly strange and terrifying. Your brain creates its own temporary visual reality.
Watch the Blood Vessels in Your Retina
In a retinal migraine, the tiny vessels in your eye suddenly tighten up. This constriction briefly cuts off the vital oxygen supply. You then lose sight on just one side. It feels quite different and scary.
The pain usually sits right behind the affected eye. It doesn’t feel like those common, dull tension-type headaches.
You can compare this to other headaches to see the difference. Knowing the exact location helps.
The mechanism is strictly vascular. It’s a completely different dynamic from the typical brain aura.
Map Your Triggers with Digital Tracking Tools
Understanding the biology is one thing, but knowing what sparks an ocular migraine aura for you is the real power.
Pinpoint Environmental Factors and Lifestyle Triggers
Bright lights often act as a fuse. Blue light from your digital smartphone screen is a frequent offender. Staying hydrated is also vital for keeping those symptoms at bay.
Atmospheric shifts often catch you off guard. Tracking unexpected migraine triggers like barometric pressure changes helps. These environmental fluctuations often go unnoticed without a consistent log.
Watch your plate closely. Certain food additives can trigger sudden visual auras without any warning.
Record every detail. Each observation helps you identify your own unique and personal migraine patterns.
Use Migraine Companion to Predict Future Attacks
Meet the Migraine Companion app. This digital tool lets you log your attacks every single day. You will spot trends that are truly invisible to the naked eye. The app analyzes your data for you.
Check out these migraine relief tips to help you find your best prevention path. Custom strategies make all the difference.
Anticipate your next crisis. Knowing what is coming reduces the intense stress linked to aura.
Take back control today. Modern technology finally makes managing your health much easier and faster.
Spot the Emergency Signs That Demand Action
While most auras are harmless, certain signs mean you must seek medical attention without waiting a single second.
Tell the Difference Between Aura and Stroke
A typical aura creeps in slowly over five to twenty minutes. Conversely, a stroke or mini-stroke strikes with brutal, instant speed. This timing difference is a vital, life-saving clue.
Correctly identifying your aura type is a vital safety measure. The American Headache Society provides great resources for patients. Stay informed to stay safe and calm.
Watch for specific emergency red flags. Weakness on one side of your body or sudden speech difficulties require an immediate ER visit.
Do not take any chances. Call emergency services immediately if you feel something is wrong.
Prevent Rare Complications and Permanent Damage
Rare complications like retinal infarction can lead to permanent vision loss. This is a very grave ocular migraine complication. Regular ophthalmological check-ups are absolutely indispensable for your safety. Never neglect these episodes.
If auras start after age 40 or 50, see a neurologist quickly. New neurological symptoms require professional medical screening.
The stress migraine link shows how tension impacts your attack frequency. Managing stress effectively helps protect your long-term vision.
Protect your precious sight. Prevention is your strongest weapon against any rare but serious damage.
Distinguishing a brain-based ocular migraine aura from rare retinal issues is vital for your safety. Perform the one-eye test and track triggers to regain control. You deserve a life without visual uncertainty. Take charge today for a clearer, pain-free tomorrow.
FAQ
What exactly is an “ocular migraine” and what are the common symptoms?
The term “ocular migraine” is actually a bit outdated and often confusing. Most doctors now use it to describe visual disturbances—like flickering lights, shimmering zigzags, or blind spots—that usually last between 5 and 60 minutes. You might see stars or colorful lines dancing across your field of vision, sometimes followed by a throbbing headache.
It is your brain’s way of signaling a neurological storm. While the symptoms feel like they are in your eyes, the source is typically a wave of electrical activity moving across your brain’s visual cortex. Disruptive? Yes. But usually, it is a temporary “glitch” in your system.
Is there a real difference between a migraine with aura and a retinal migraine?
Yes, and the distinction is vital. A migraine with aura is the most common type, where the visual “show” happens in both eyes simultaneously because it originates in the brain. If you close your eyes or cover one, the zigzags remain. It is a neurological event.
A retinal migraine is much rarer and affects only one eye. This happens when blood vessels in the eye itself constrict, briefly cutting off oxygen to the retina. Use the “one-eye test”: cover the affected eye. If the symptoms disappear, the problem is likely retinal and requires specific medical attention.
Can these visual disturbances be dangerous or lead to a stroke?
While most auras are harmless, you must watch the clock. A typical migraine aura develops gradually over five minutes or more. In contrast, a stroke or mini-stroke usually strikes suddenly and without warning. This “suddenness” is a major red flag that demands immediate action.
Seek emergency care if you experience a “curtain” falling over your vision, sudden weakness on one side of your body, or difficulty speaking. These are not typical migraine symptoms. Never ignore a sudden neurological change. Your safety depends on a quick response.
What are the most common triggers for these visual migraine attacks?
Your lifestyle and environment are often the hidden culprits. High-frequency triggers include dehydration, flickering blue light from digital screens, and sudden spikes in stress. Even something as simple as a glass of red wine or a change in weather pressure can set off an episode.
Identifying your personal patterns is the first step toward relief. Many sufferers find that tracking their daily habits helps them predict and prevent future attacks. Small changes, like better sleep hygiene and staying hydrated, can significantly reduce the frequency of these frightening visual “auras.”
How can I manage a migraine aura when it starts?
When the shimmering starts, the best move is to find a dark, quiet space immediately. Since the brain is over-excited, reducing sensory input—like bright lights and loud noises—can help the wave pass more comfortably. Applying a cool compress to your forehead may also provide soothing relief.
Don’t wait for the pain to hit. Using digital tools like Migraine Companion can help you log the event and choose the best management strategy. Taking control of your data turns fear into a proactive plan for recovery.
Why do I sometimes get the visual “aura” without any headache at all?
This is a common phenomenon known as an “acephalgic” or “silent” migraine. You experience the full visual display—the flashes, the zigzags, or the blind spots—but the expected pain never arrives. It is still a migraine event; your brain simply skipped the headache phase this time.
While a silent migraine is a relief in terms of pain, it still signals that your brain is reacting to a trigger. It is important to document these episodes just as you would a painful one. Understanding your brain’s unique language is key to long-term health management.