The key takeaway: Migraines are a neurological disease, not just headaches, affecting 1 in 5 women and 1 in 16 men. Recognizing the four phases—prodrome, aura, attack, postdrome—and triggers like stress or hormonal changes empowers proactive management. Understanding its genetic basis and symptom complexity helps reduce disability and improve treatment outcomes.
Are you tired of confusing migraines with ordinary headaches, only to feel overwhelmed by symptoms like pulsating pain, light sensitivity, nausea, or post-attack fatigue? This article demystifies migraine symptoms causes, explaining their progression through four phases—from early warning signs (mood shifts, neck stiffness) to the headache phase and “migraine hangover.” Rooted in neurological factors like genetic predispositions, hormonal changes, and brain chemical imbalances (serotonin, CGRP), migraines affect 1 in 5 women and 1 in 16 men. Explore expert-backed insights into hidden triggers (diet, weather shifts, sensory overload) and actionable strategies to identify patterns, helping you take control of this widespread, misunderstood condition.
- What is a migraine? more than just a headache
- The Four Phases of a Migraine Attack
- Unraveling the Deep-Rooted Causes of Migraine
- Common migraine triggers you should know
- Who is most at risk? key migraine risk factors
- Beyond the headache: the broader impact of migraine
- When to see a doctor for your headaches

What is a migraine? more than just a headache
Imagine waking up with a headache so intense that even the softest light feels unbearable. This is the reality for millions suffering from migraines, often mistaken for ordinary headaches. Did you know 90% of sufferers experience moderate to severe pain impacting daily life? Understanding migraine as neurological disease reveals its complex nature.
A migraine isn’t just head pain. It’s a neurological disease rooted in genetics, involving brain chemical imbalances and nerve pathway changes. While headaches cause generalized pain, migraines typically present as pulsating, one-sided discomfort. The Cleveland Clinic confirms this pain becomes so severe that 73% of patients struggle completing basic tasks during attacks.
Affecting 1 in 5 women, 1 in 16 men, and 1 in 11 children globally, migraines transcend typical head pain. They bring nausea, light sensitivity, and sound intolerance. The World Health Organization classifies severe migraines as among the world’s most disabling conditions, outranking diabetes and asthma in disability impact.
These attacks progress through four phases. The prodrome phase gives early warning signs like mood shifts. Aura brings visual disturbances for 1/3 of patients. The attack itself lasts 4-72 hours, followed by a postdrome “hangover” phase. This complexity explains why 60% of sufferers report family history – it’s not just a bad day.
The Four Phases of a Migraine Attack
Why do some migraines strike suddenly while others build gradually? The answer lies in understanding the four distinct phases that shape these attacks. Recognizing these patterns transforms how you manage migraines. This resource explains how tracking phases can predict and potentially prevent full attacks.
Phase 1: The Prodrome (The Warning Signs)
Your body might send signals up to 48 hours before pain hits. The prodrome phase acts as an early warning system. Common indicators include:
- Extreme mood shifts – from sudden euphoria to irritability
- Neck tension that feels like a tightening vice
- Unusual cravings (often misinterpreted as triggers)
- Excessive thirst or frequent urination
- Uncontrollable yawning without tiredness
Many mistake these changes for stress. Research shows 60% of migraineurs overlook prodrome symptoms. Catching these early signals creates a 12–24 hour window for action – like magnesium supplements or strategic rest. Think of it as spotting storm clouds before the storm. Importantly, recognizing prodrome symptoms can reduce attack severity by up to 30% when treated early.
Phase 2: The Aura (Sensory Disturbances)
For 30% of sufferers, visual warnings appear 5–60 minutes before pain. These neurological symptoms include:
- Visual: Zigzag lines, shimmering blind spots (ScienceDirect)
- Sensory: Tingling starting in one hand and spreading up an arm
- Speech: Temporary word-finding difficulties
Behind these symptoms lies cortical spreading depression – a wave of brain activity that temporarily disrupts function. Some experience “silent migraines” with aura but no pain, creating confusion. Recognizing patterns helps distinguish neurological warnings from random sensations. For instance, visual disturbances often start in one eye and spread, while sensory issues typically affect one side of the body.

Phase 3: The Attack (The Headache Phase)
This is the phase most recognize as “the migraine.” Key characteristics include:
- Debilitating, pulsating pain – often one-sided
- Nausea or vomiting in 80% of cases
- Extreme sensitivity to light/sound – even dim light feels blinding
- Pain worsening with movement
Untreated attacks last 4–72 hours. Picture trying to work while wearing migraine-inducing sunglasses and noise-cancelling headphones playing static, all with head pressure. This explains why 90% can’t work during attacks. The pain stems from inflamed meninges activating pain receptors – making even gentle touch agonizing. Unlike regular headaches, migraines involve CGRP release, which explains their intensity and associated symptoms.
Phase 4: The Postdrome (The Migraine Hangover)
After pain fades, up to 80% experience “migraine hangovers” (Harvard Health). This recovery phase brings:
- Brain fog – forgetting why you walked into a room
- Physical exhaustion despite rest
- Emotional shifts – from euphoria to fatigue
- Neck pain returning with sudden movements
| Phase | Typical Duration | Key Symptoms |
|---|---|---|
| Prodrome | 1–2 days before | Mood changes, neck stiffness, cravings, frequent urination |
| Aura | Up to 60 minutes | Visual disturbances, tingling, speech difficulty |
| Attack | 4–72 hours | Throbbing pain, nausea, light/sound sensitivity |
| Postdrome | 1–2 days after | Fatigue, confusion, “washed out” feeling |
This neurological recovery explains feeling “hungover” without alcohol. Your brain remains hypersensitive as it resets. Treat it like post-surgery recovery – gentle movement, hydration, and strategic caffeine use can ease the transition. Harvard research shows keeping a headache journal during postdrome helps identify recovery patterns. Missing this phase in management plans means missing half the battle – 40% report residual symptoms affecting next-day productivity.
Unraveling the Deep-Rooted Causes of Migraine

The Role of Genetics and Brain Chemistry
Migraines are complex neurological events, not just severe headaches. Up to 80% of sufferers have a close relative with the condition (Cleveland Clinic), proving genetics matter. If one parent has migraines, their child has a 50-75% chance of developing them. Specific genes like CACNA1A and ATP1A2 are linked to familial hemiplegic migraine (FHM), a rare subtype where ion channel mutations make neurons hyper-responsive to stimuli like stress or sensory overload.
Chemical imbalances in the brain act as hidden triggers. Serotonin regulates pain signals. When levels drop—due to stress, skipped meals, or hormonal shifts—blood vessels dilate, potentially sparking migraines. Low serotonin also amplifies pain perception, turning minor discomforts into crises. For example, low blood sugar from missed meals can trigger serotonin dips, explaining why regular eating habits matter for migraine management.
The CGRP protein (Calcitonin Gene-Related Peptide) is critical. During migraines, CGRP floods the nervous system, causing inflammation and widening brain blood vessels. CGRP levels spike during attacks, and infusions can trigger migraine-like symptoms. Monoclonal antibody treatments targeting CGRP show promise, proving its central role. Researchers even measure CGRP in saliva and tears—non-invasive methods—to study migraine activity, though its short half-life (7–9 minutes) complicates tracking.
Brain Activity and the Trigeminal Nerve
The trigeminal nerve—your largest pain sensor—becomes overactive during migraines. Abnormal electrical waves in the brainstem activate this nerve, releasing CGRP and other chemicals that amplify pain. Light, sound, or touch suddenly feel intolerable. The brainstem’s misfiring misinterprets normal inputs as painful, creating a cycle: nerve activation → CGRP release → inflamed vessels → intensified pain.
Signals travel from the trigeminal nerve to the brainstem’s trigemino-cervical complex, then to the thalamus—a pain signal relay station—and finally to cortical regions responsible for pain perception. This explains why migraines feel like a full-body assault. The thalamus acts as a filter for sensory input; when overwhelmed, it becomes a hub for migraine symptoms like light sensitivity or nausea.
Understanding these mechanisms shows migraines are more than headaches—they’re neurological chain reactions. By decoding genetics, brain chemistry, and nerve pathways, we can develop targeted interventions to break the cycle at its source. For deeper insights into genetic links, explore more about migraine triggers.
These biological processes underscore why migraines are hereditary for many. They also explain why lifestyle factors—like diet, sleep, and stress—play roles in prevention. Future therapies may target gene regulation or CGRP pathways to stop migraines before they start, transforming how we manage this condition.
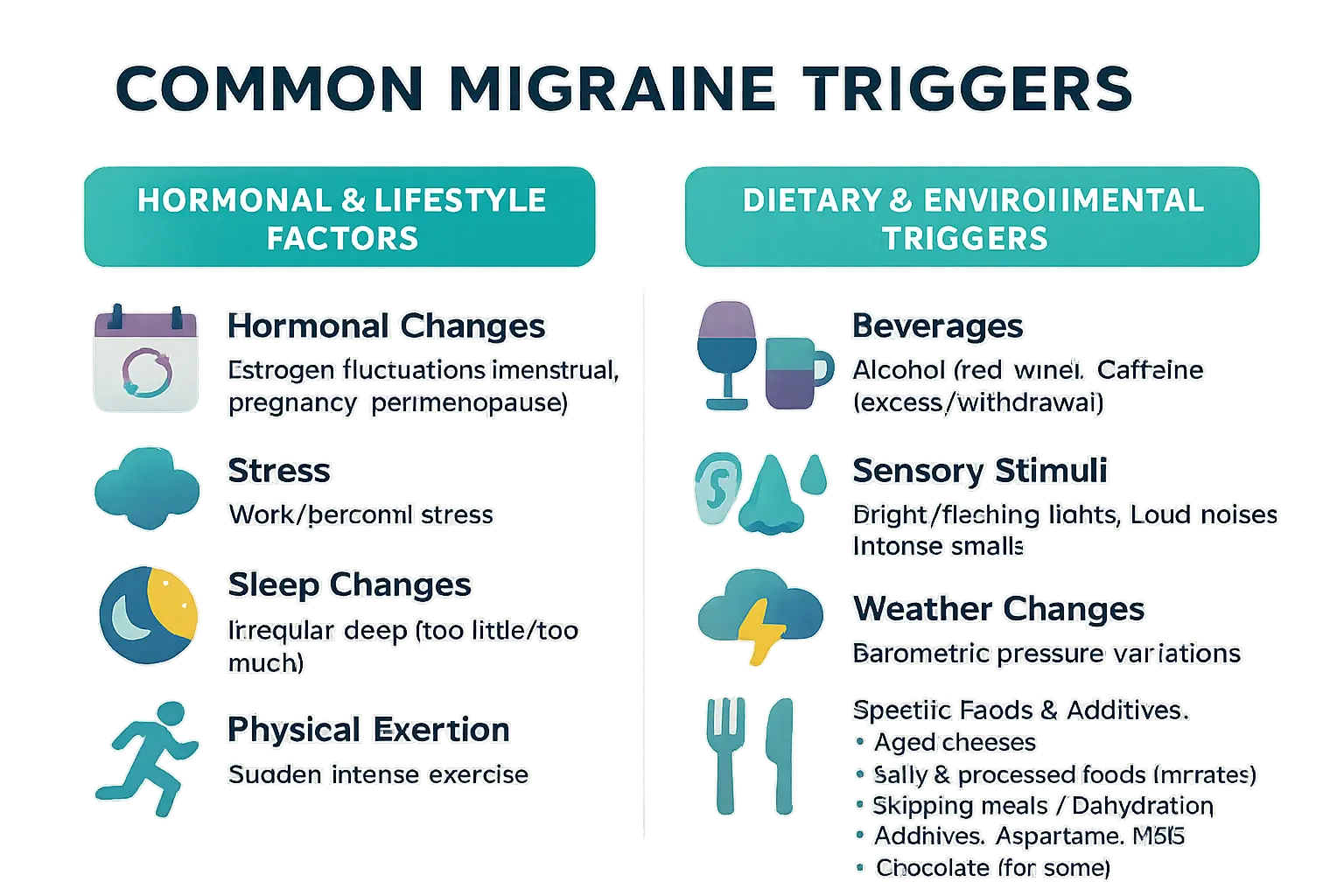
Common migraine triggers you should know
Hormonal and lifestyle factors
Migraines disproportionately affect women, with 1 in 5 women experiencing them compared to 1 in 16 men. This gender gap stems largely from estrogen’s influence. Fluctuations in this hormone, especially the sudden drop before menstruation, sensitize brain pathways. ScienceDirect explains how this estrogen withdrawal increases pain sensitivity during menstrual cycles, pregnancy shifts, or perimenopause.
Stress acts as a double-edged sword. While short-term stress can mask migraines through cortisol release, the “let-down” period after stress subsides becomes dangerous. Cortisol changes trigger up to 70% of migraine attacks, creating what researchers call “stress let-down headaches.” Physical stress like irregular sleep patterns proves equally risky – both 3 a.m. wakeups and weekend lie-ins disrupt the brain’s delicate balance.
Physical exertion creates unexpected risks. Intense exercise triggers migraines in 10% of sufferers through sudden blood flow changes. Even sexual activity, which causes temporary blood pressure spikes, activates migraines in sensitive individuals. Sleep disturbances affect half of migraineurs, with both insomnia and oversleeping creating vulnerability by altering neurotransmitter levels like serotonin.
Dietary and environmental triggers
Food triggers work through complex chemistry. Aged cheeses contain tyramine, an amino acid that constricts blood vessels and affects brain signaling. Processed meats with nitrates convert to nitric oxide, dilating blood vessels and activating pain receptors. Missed meals trigger migraines through blood sugar crashes and dehydration, which affects brain tissue hydration levels.
Environmental sensitivity creates daily challenges. 80% of sufferers react to sensory overload – fluorescent lighting’s imperceptible flicker, sudden loud noises, or strong perfumes. Weather changes prove surprisingly potent: 50% of migraineurs react to barometric pressure shifts, high humidity, or temperature spikes. These changes affect blood flow and brain chemistry.
Consider these common triggers:
- Alcohol (especially red wine) combines histamines, sulfites, and dehydration effects
- Caffeine’s paradox – 200mg daily helps some, while 1 day without causes withdrawal headaches
- Strong smells from paint thinner to perfume overstimulate olfactory nerves
- Sunlight glare or computer screen flicker overactivate visual cortex
- Weather changes like approaching storms alter atmospheric pressure
- Dehydration reduces blood volume, making brain tissue temporarily shrink
Triggers rarely work alone. Like a chain reaction, combinations matter most. The “perfect storm” might include estrogen drop + 3 hours sleep + skipped breakfast + red wine. This explains why trigger diaries matter – recording 200+ factors in 80% of cases reveals patterns.
Understanding these connections transforms migraine management. For hormonal triggers, tracking cycles helps anticipate vulnerable periods. For dietary triggers, elimination diets identify personal sensitivities. Environmental awareness means bringing sunglasses indoors for fluorescent lights. The goal isn’t total avoidance, but creating a personalized migraine defense system that reduces frequency by 40-50% through lifestyle adjustments.
Remember, your migraine fingerprint is unique. While one person might handle wine but not chocolate, another sees migraines after both. The key lies in gradual experimentation: remove potential triggers for 4-6 weeks, then reintroduce systematically while tracking responses. This scientific approach turns migraine management from chaos into control.
Who is most at risk? key migraine risk factors
Migraines follow predictable patterns – specific risk factors identify who’s more susceptible. Unlike triggers causing attacks, these factors create biological vulnerability. Recognizing them enables prevention without undue alarm, as risks don’t guarantee symptoms. Migraine Quebec reports 1 in 5 women and 1 in 16 men live with migraines, revealing clear gender differences.
- Family history: Genetics weigh heavily. If one parent has migraines, children face 40-50% risk; both parents increase it to 75%. Twin studies show 80% heritability – genetics are the strongest risk factor, though environment influences symptom expression.
- Age: Migraines often strike during hormonal transitions – adolescence sees first attacks, peak impact hits adults in their 30s. Though symptoms often ease post-menopause, 1 in 11 children experience migraines, confirmed by the American Migraine Foundation.
- Sex: Hormonal shifts drive disparities. Estrogen fluctuations during menstrual cycles, pregnancy, or menopause correlate with attacks. Harvard Health Publishing notes hormonal contraceptives worsen symptoms. Adult women face threefold higher rates than men despite equal childhood prevalence.
- Medical conditions: Comorbidities compound risks. WHO data shows 25% of migraineurs also battle depression/anxiety – double the general population. Sleep disorders increase migraine risk 2-4 times, while epilepsy patients face 2-3x higher rates, suggesting shared neurological vulnerabilities.

Recognizing these factors transforms migraines from random events into predictable patterns. It enables monitoring for at-risk groups like teens in hormonal flux or adults with mood disorders. However, risk factors aren’t destiny. They act like weather alerts – preparing without predicting inevitable attacks. Understanding these blueprints empowers prevention before migraines establish their foothold.
Beyond the headache: the broader impact of migraine

The link between nutritional deficiencies and migraine
Migraines aren’t just about head pain. Emerging research suggests nutritional deficiencies might play a role in triggering episodes. Three key nutrients—magnesium, riboflavine (vitamin B2), and Coenzyme Q10 (CoQ10)—are frequently linked to migraine management.
Magnesium helps regulate nerve function and may reduce brain hyperexcitability, a known migraine driver. Studies show some migraine patients have lower magnesium levels. While not a cure, discussing supplementation with a doctor could be beneficial.
- Riboflavin supports mitochondrial energy production, potentially addressing energy deficits in migraine-prone brains.
- CoQ10, an antioxidant, aids cellular energy and reduces inflammation tied to migraine pathways.
These supplements aren’t standalone solutions. Their effectiveness varies, and professional guidance is critical—especially during pregnancy or when taking other medications. Tracking symptoms in a headache journal helps assess their impact over 2-3 months.
Migraine’s toll on mental health and daily life
The ripple effects of migraines extend far beyond physical pain. During the interictal period (time between attacks), 41.5% of patients experience lingering symptoms like light sensitivity or brain fog, according to Japanese studies. This constant “wait-for-the-next-attack” anxiety creates invisible stress.
Chronic migraine sufferers often face a double burden: 2-4 times higher risk of anxiety and depression compared to the general population. The Migraine Interictal Burden Scale (MIBS-4) reveals how this hidden toll diminishes work productivity, social connections, and emotional well-being.
Daily life becomes a minefield of compromises. Simple tasks like grocery shopping or attending meetings may trigger attacks due to light/sound sensitivity. Imagine canceling plans last-minute 15% of the time—this unpredictability strains relationships and career growth. For practical strategies, explore tools to manage migraine’s daily impact.
Neurological research shows migraine brains remain hyper-responsive between attacks, explaining why stress management and preventive care matter. This understanding shifts migraine from being “just a headache” to a complex condition requiring holistic management.

When to see a doctor for your headaches
If you suspect migraines, seeking medical advice is crucial. A diagnosis from a healthcare professional clarifies your condition and opens doors to personalized management strategies. Migraines are complex—they’re not just headaches but neurological events with symptoms like light sensitivity, nausea, and aura.
Changes in your headache pattern demand attention. Did your migraines start feeling different? Are they more frequent or severe? These shifts could signal underlying issues. Even if you’ve managed migraines before, new developments warrant a check-up.
Not all headaches require immediate action, but certain red flags shouldn’t be ignored. Here’s what to watch for:
- A sudden, excruciating headache—often described as a “thunderclap.” This could signal a brain hemorrhage or aneurysm.
- Fever with neck stiffness, confusion, or seizures. These might indicate meningitis or encephalitis.
- New neurological symptoms like vision loss, speech difficulties, or paralysis, which could point to a stroke.
- Head trauma followed by a headache. Even minor impacts can cause delayed complications.
These symptoms need urgent care. Call emergency services if you experience them. For less urgent concerns, consult your doctor to refine your prevention plan. Understanding your triggers and symptoms empowers you to reduce their impact. With professional guidance, managing migraines becomes a structured journey, not a guessing game.
Remember: early intervention prevents escalation. Your health is worth prioritizing.
Migraine is a neurological disorder beyond a headache, with varied symptoms and triggers. Understanding your experiences, identifying triggers, and seeking medical advice are key to effective management. With proper support and adjustments, you can reduce their impact and enhance life quality. Consult a healthcare professional to manage migraines confidently.
FAQ
What causes migraines?
Migraines result from a combination of genetic and environmental factors. Research shows up to 80% of migraine sufferers have a close relative with the condition, indicating strong genetic component (Cleveland Clinic). The underlying causes involve changes in brain chemistry, particularly serotonin levels which regulate pain, and calcitonin gene-related peptide (CGRP), a protein involved in pain transmission and brain vessel inflammation. Brain activity affecting the trigeminal nerve, a major pain pathway for the face and head, also plays a role. While these are the fundamental causes, specific “triggers” like hormonal changes, stress, certain foods, and sensory stimuli can provoke individual attacks.
Is there a definitive cure for migraines?
While there’s no universal “cure” for migraines, effective management strategies exist. Treatment focuses on two approaches: acute treatment to stop attacks when they occur, and preventive treatment to reduce frequency and severity. Acute treatments include over-the-counter pain relievers (ibuprofen, aspirin), prescription medications like triptans, and newer CGRP receptor antagonists. Preventive approaches might involve daily medications (beta-blockers, anti-seizure drugs), lifestyle modifications, and neuromodulation devices. Many people find significant relief through personalized treatment plans developed with their doctors, combining medication with lifestyle adjustments.
What are the stages of a migraine attack?
Migraine attacks typically progress through four stages, though not everyone experiences all of them:1. Prodrome (pre-headache phase): Occurs 1-2 days before, with subtle changes like mood swings, neck stiffness, food cravings, and frequent yawning.2. Aura: Visual disturbances (flashing lights, blind spots), sensory changes (tingling), or speech difficulties that develop gradually over 5-60 minutes.3. Attack: The actual headache phase with throbbing pain lasting 4-72 hours, often accompanied by nausea, light/sound sensitivity, and movement sensitivity.4. Postdrome: “Migraine hangover” affecting up to 80% of sufferers, with fatigue, confusion, or body aches lasting 1-2 days. (Harvard Health Publishing)
What are the most effective migraine treatments?
Treatment effectiveness varies by individual, but we have several proven approaches:For acute treatment: Triptans (sumatriptan, rizatriptan) target serotonin receptors and are most effective when taken early. CGRP antagonists (ubrogepant, rimegepant) represent newer options with fewer cardiovascular concerns. NSAIDs like ibuprofen or naproxen work well for mild to moderate attacks.For prevention: Beta-blockers (propranolol), anticonvulsants (topiramate), and newer CGRP monoclonal antibodies (erenumab) show good efficacy. Non-pharmacological approaches like biofeedback, cognitive behavioral therapy, and regular exercise complement medication. Emerging evidence supports neuromodulation devices that use electrical or magnetic stimulation.
What provides quick relief during a migraine attack?
For fast relief, act early when the headache is still mild. Take your prescribed acute medication (like triptans or CGRP antagonists) with water, then rest in a dark, quiet environment. Some find cold compresses on the forehead or neck helpful. For severe cases, injectable sumatriptan works within 10-15 minutes. Stay hydrated and consider anti-nausea medications if vomiting occurs. Early treatment improves medication effectiveness – don’t wait until pain becomes severe.
Can migraines indicate other health issues?
Migraines themselves are primary neurological disorders, but they can co-occur with other conditions. They’re associated with increased stroke risk, particularly in women with migraine with aura. Migraines often co-exist with depression, anxiety, sleep disorders, and epilepsy (World Health Organization). Thunderclap headaches (sudden, severe) or new neurological symptoms (vision loss, speech problems) might indicate other issues – these require immediate medical evaluation. Most migraines aren’t symptoms of other diseases, but they’re associated with various health conditions.
Which vitamin deficiencies might contribute to migraines?
Research suggests certain nutrient deficiencies may play roles in migraines:- Magnesium deficiency might increase brain excitability and CGRP release- Riboflavin (vitamin B2) deficiency could impair mitochondrial function- Coenzyme Q10 deficiency affects cellular energy production. While not everyone with migraines has these deficiencies, supplements have shown preventive benefits in clinical studies. Magnesium (400-600 mg/day), riboflavin (400 mg/day), and CoQ10 (100-300 mg/day) have demonstrated effectiveness in reducing migraine frequency, though individual responses vary.
When should someone seek emergency care for migraine?
Seek immediate medical attention for:- A sudden, extremely severe headache (thunderclap headache)- Headache with fever, neck stiffness, confusion, or seizures- New neurological symptoms (vision loss, speech problems, weakness)- Headache after head traumaThese “red flags” might indicate more serious conditions like stroke or meningitis. Also consult a doctor if your headache pattern changes, attacks worsen, or usual treatments stop working. Regular ER visits shouldn’t be necessary for typical migraines with established treatment plans.
What are the 5 C’s of migraines?
While we commonly discuss the four phases of migraine (prodrome, aura, attack, postdrome), the “5 C’s” framework isn’t standard terminology in migraine science. However, we can consider five key migraine characteristics:1. Complex – Involving multiple brain systems and neurotransmitter imbalances2. Chronic – For some, progressing to chronic migraine (15+ headache days/month)3. Cyclical – Following predictable patterns in many individuals4. Comorbid – Frequently occurring with depression, anxiety, and other conditions5. Controllable – With proper diagnosis and personalized treatment plans
