Ever wondered why a glass of wine or a stressful day can unleash a migraine? Migraine triggers—like hormonal shifts, dietary factors, or sensory overload—act as personal “switches” that ignite attacks in those genetically predisposed. Unlike root causes (genetic and neurological), triggers vary widely and accumulate, like drops in a bucket, until the migraine threshold is crossed. This article explains the science, why your unique biology matters, and how tracking patterns—sleep, hydration, stress—can help. According to a 2023 Journal of Headache Research study, nearly all of patients have multiple triggers. Learn how small, evidence-based adjustments could reduce attack frequency and reclaim control.
- What are migraine triggers? (and what they are not)
- The Science Of Triggers: Understanding Your Personal Migraine Threshold
- The most common categories of migraine triggers
- Decoding Dietary Triggers: Foods, Drinks, and Additives
- Trigger or symptom? The truth about prodrome cravings
- The hidden factor: How nutritional deficiencies can affect your migraines
- Your best tool: How to identify your personal triggers with a migraine diary
- From Identification to Action: Creating Your Trigger Management Strategy
What are migraine triggers? (and what they are not)

Migraines are complex neurological events rooted in genetics and brain function. But what activates them? The answer lies in migraine triggers – specific factors that act like switches for your pain. Let’s clarify what these triggers are, what they aren’t, and why this distinction matters for managing your health.
Triggers vs. causes: the critical difference
Triggers aren’t the same as causes. Migraine is a neurological disease with genetic roots – your brain processes stimuli differently. Triggers are external or internal factors that activate this vulnerability. Think of it like a gun: your neurological makeup is the loaded chamber, while triggers are what pull the trigger.
Blaming yourself for triggers misses the point. Skipping breakfast didn’t cause your migraines – it simply activated a pre-existing condition. This distinction shifts focus from guilt to empowerment.
Why your “trigger” might not be mine
Why does the same food, weather, or stressor affect people differently? A 2023 study in Cephalalgia found nearly 100% of participants had identifiable triggers, but no single factor affected everyone. Some react to chocolate, others to pressure changes. Your unique neurological fingerprint determines which switches get flipped.
Tracking triggers: your roadmap to control
Identifying personal triggers isn’t about deprivation – it’s about clarity. When you understand your activators, you can make strategic choices to reduce crisis frequency and severity. For example, if sleep disruptions are your primary activator, prioritizing consistent sleep hygiene becomes powerful. This isn’t perfection – it’s pattern recognition to take control of your health.
The Science Of Triggers: Understanding Your Personal Migraine Threshold
Migraine Threshold Explained
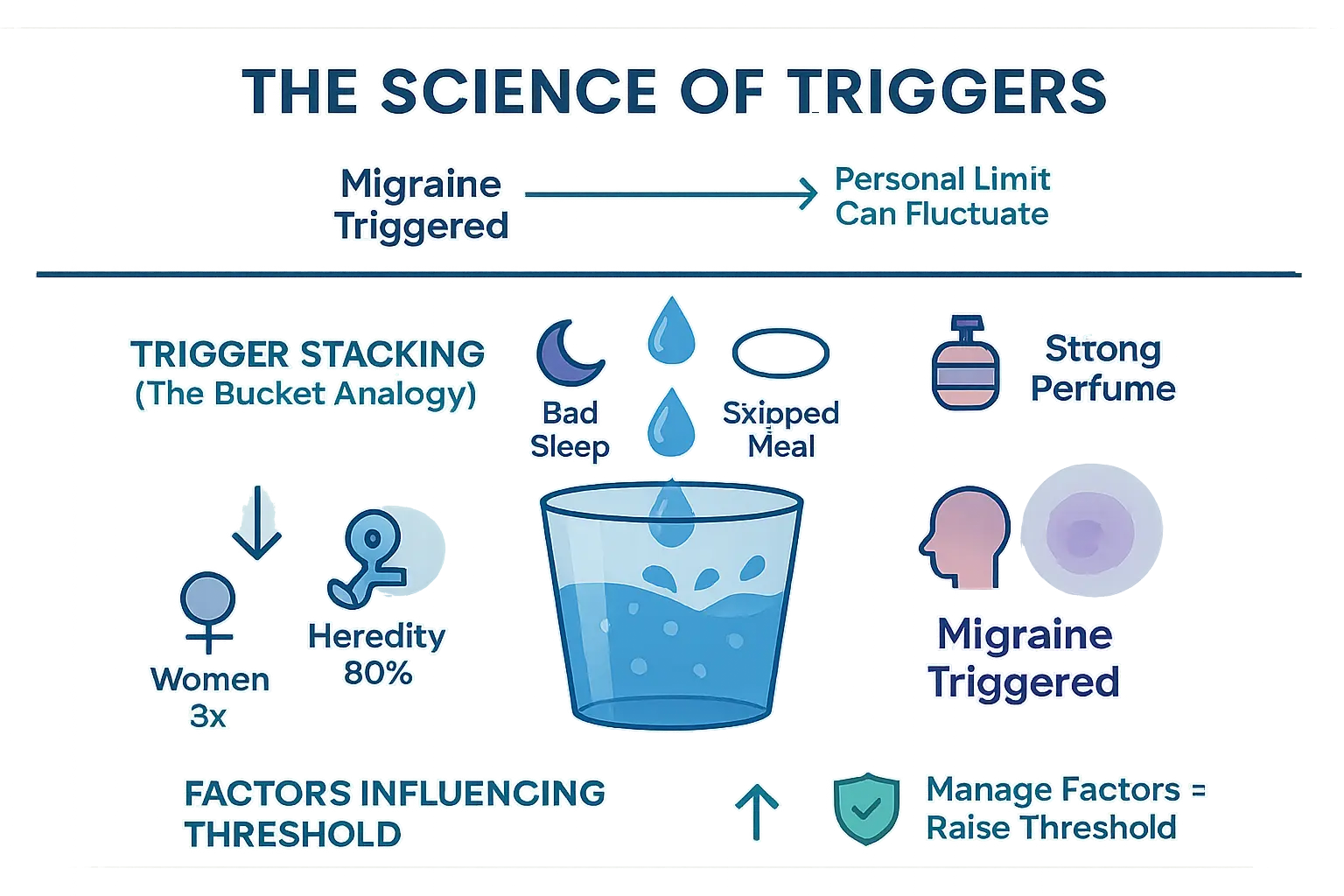
Imagine your brain as a container holding stress, fatigue, and irritants. The migraine threshold represents how much your nervous system can tolerate before a crisis occurs. When these “stress drops” exceed your personal limit, a migraine starts. This threshold isn’t fixed – it shifts with factors like hormonal cycles, sleep quality, and baseline stress levels. For example, a busy workweek might lower your threshold, making you more vulnerable to sensory overload. During menstruation, estrogen drops can temporarily shrink this buffer zone, explaining why some women experience migraines at specific cycle phases.
Trigger Stacking: The Drop Effect
Migraines often result from multiple triggers combining rather than single causes. Consider this: one night of poor sleep (1st drop) + skipped breakfast (2nd) + perfume exposure (3rd) might overwhelm your system. This “trigger stacking“ explains why identical situations don’t always produce migraines. Like filling a bucket drop by drop, the final trigger might seem minor yet push you past your limit. This cumulative effect makes tracking patterns essential for prevention. For instance, a rainy day might not cause issues alone, but combined with sleep deprivation and weather pressure changes, it becomes a perfect storm.
Factors Shaping Your Sensitivity
Three key elements influence this delicate balance:
- Genetics – 80% of sufferers have family history, with women 3x more affected than men. Specific genes like CACNA1A (linked to calcium channels) and TRESK mutations demonstrate inherited sensitivity.
- Hormonal shifts – Estrogen fluctuations explain menstrual migraines and sensitivity changes across life stages. During menopause, 62% of women report reduced frequency as hormonal volatility decreases.
- Baseline health – Anxiety, sleep disorders, and chronic stress create a more reactive nervous system. Poor sleep disrupts pain regulation, while anxiety increases cortical excitability, both lowering your personal threshold.
Understanding these factors reveals why prevention works better than reaction. By maintaining regular sleep, hydration, and stress management, you effectively “raise the bucket’s height” – creating more buffer against inevitable triggers. This personalized approach forms the foundation for effective migraine management. For example, consistent sleep patterns can increase your threshold by 20-30%, while proper hydration improves cerebral blood flow regulation. Combining these strategies creates measurable protection against environmental stressors like weather changes or workplace stress.
The most common categories of migraine triggers
- Stress and emotions
- Sleep patterns
- Hormonal fluctuations in women
- Environmental factors
- Sensory stimuli
Stress and emotions
Stress remains one of the most frequent triggers, with up to 80% of patients identifying it as a cause. This mechanism involves the release of chemical substances such as cortisol and CGRP (Calcitonin Gene-Related Peptide), which sensitize the nervous system.
The “let-down headache” hypothesis suggests that a sudden drop in stress after an intense period increases the risk of migraine up to 18 hours later. This decrease in glucocorticoids may disrupt the brain’s balance.
To manage stress, practices such as daily meditation (shown to reduce cortisol levels by 25% in a 2022 study) or biofeedback (40% effectiveness according to a 2023 meta-analysis) can help lower migraine frequency. Regular walking (30 minutes per day) also reduces episodes by 20–30%, according to Migraine Quebec.
Sleep patterns
Sleep disturbances trigger up to 50% of migraines, with a peak of attacks occurring during or right after sleep. Irregular sleep–wake cycles disrupt the production of serotonin and melatonin, two key neurotransmitters.
Both sleep deprivation (<3h per night) and excessive sleep (>9h) can trigger migraines. The well-known “weekend migraine” often appears after sleeping in for more than 2 hours, which alters cerebral homeostasis.
A strict sleep routine improves symptoms in 60% of cases, according to a 2023 study. Recommended strategies:
- Go to bed and wake up at consistent times (±30 minutes)
- Get morning exposure to natural light
- Avoid screens 2 hours before bedtime
Hormonal fluctuations in women
Around 70% of women with migraines report a connection with their menstrual cycle. The drop in estrogen levels before menstruation (below 45–50 pg/mL) triggers 20–30% of menstrual migraines, which tend to be more intense and resistant to treatment.
Combined contraceptives (estrogen + progestin) worsen migraines in 30% of users, especially when the estrogen dose exceeds 30 μg. In contrast, progestin-only contraceptives do not carry this risk.
To help reduce hormone-related migraines:
- Use low-dose estrogen pills (<20 μg)
- Prevent sudden hormonal drops with an estrogen patch during the pill-free week
- Prefer non-hormonal methods (copper IUD or progestin-only options)
Environmental factors
Weather changes trigger about 33% of migraines, with peaks occurring during shifts in barometric pressure (±5 hPa) or humidity above 70%. A Japanese study involving 15,000 patients demonstrated a 25% increase in migraine attacks during storms.
Intense sunlight (>100,000 lux) activates the extrastriate visual cortex, worsening photophobia. Heat waves (temperature >25 °C) increase headache occurrence by 7% per additional degree, according to a 2022 analysis.
Managing weather-related triggers:
- Use weather forecast apps to anticipate migraine risk
- Wear tinted glasses in strong sunlight
- Increase hydration during hot conditions
Sensory stimuli
Sensory hypersensitivity affects up to 90% of people with migraines.
Photophobia (light intolerance) can occur even between attacks, due to abnormal activation of the visual cortex. Sounds above 85 dB (equivalent to a vacuum cleaner) trigger migraines in 45% of cases.
Strong smells—such as perfumes containing lavender or vanillin—activate the amygdala and hippocampus, triggering migraines in 30% of patients. Monosodium glutamate (E621) found in processed foods can worsen these reactions.
Prevention of sensory triggers:
- Wear blue-light filtering glasses (reduces light-induced migraines by 40%)
- Use noise-reduction earplugs (attenuation of 25–30 dB)
- Avoid environments with strong odors (perfumeries, industrial kitchens)
Decoding Dietary Triggers: Foods, Drinks, and Additives
Why Meal Regularity Matters
Skipping meals destabilizes brain glucose levels. Your brain uses 20% of daily glucose despite being 2% of body weight. Hypoglycemia triggers migraines in 40-70% by activating stress hormones. Migraine Quebec warns against intermittent fasting, causing cerebral glucose deprivation in 40% of users.
Hydration matters: 2% dehydration reduces cerebral blood flow by 13%. The 1.5L daily intake requires timed sipping with meals to avoid osmotic shock. Caffeinated drinks cause 1.5x fluid loss versus water, creating a paradoxical risk.
Common Culprits and Their Paradoxes
Red wine’s triple threat combines tyramine, ethanol’s vasodilation, and dehydration. French Migraine Society data shows 77% react within 3 hours of consumption, often with second-day rebound.
Caffeine’s dual role appears in 150mg chocolate bars. While used in painkillers, overuse causes 9.4% of chronic cases. Weekend migraines often follow reduced weekday intake.
Aged cheese tyramine increases from 6mg/100g (cheddar) to 400mg/100g (parmesan). Sensitivity varies by COMT gene variants.
Hidden Additives to Monitor
- Monosodium Glutamate (MSG) appears in 47% of prepared meals exceeding EU limits. La Voix des Migraineux notes reactions correlate with portion size.
- Aspartame’s 28% European prevalence includes unexpected sources. Animal studies show gut dysbiosis at high doses, but human links remain speculative.
- Nitrates/Nitrites in processed meats create nitrosamines linked to cancer risks. Vegetable nitrates lack these risks due to polyphenol protection.
Practical Substitution Guide
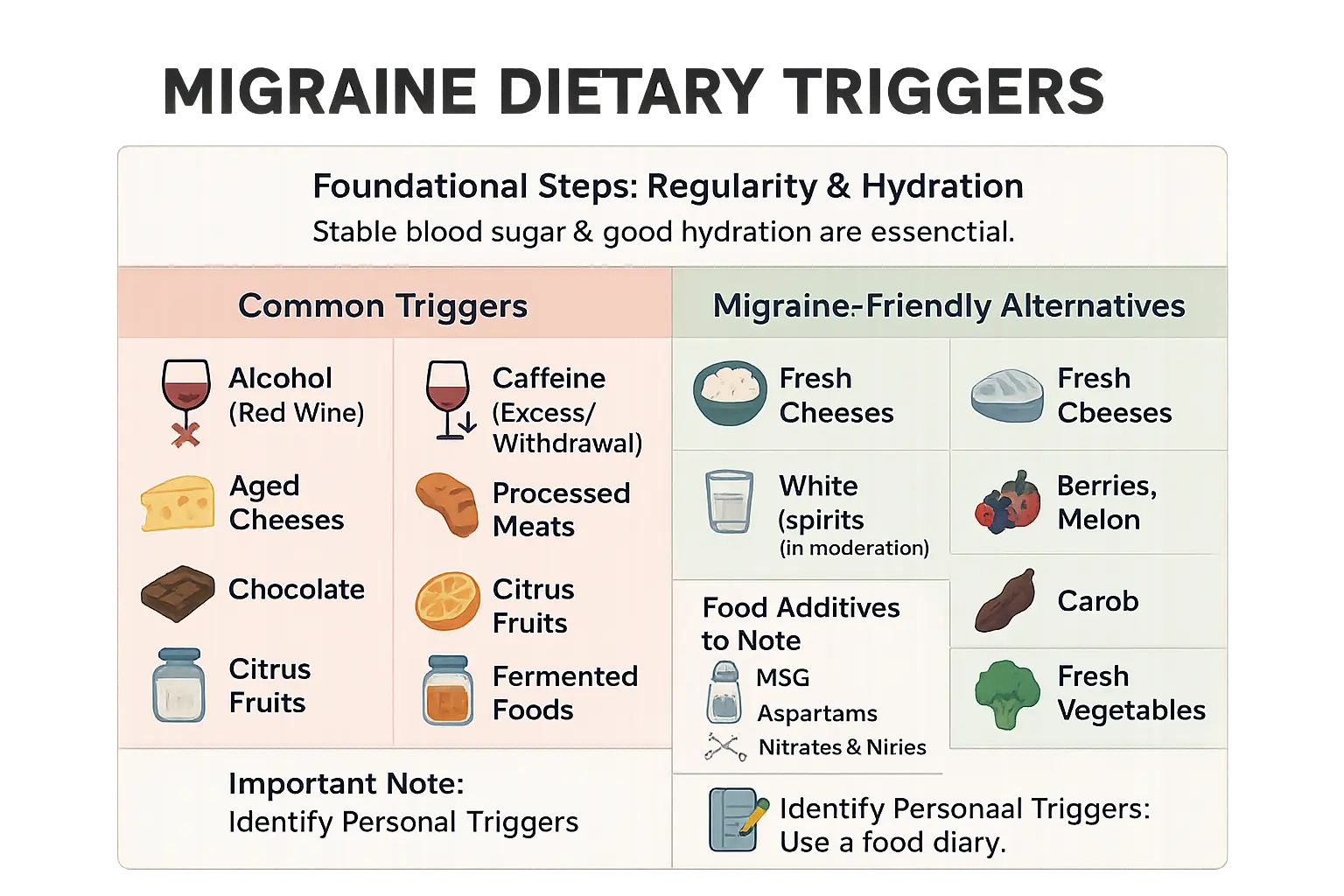
| Common Trigger | Potential Migraine-Friendly Alternative |
|---|---|
| Aged cheeses (Cheddar, blue cheese, brie) | Fresh cheeses (ricotta, cottage cheese, cream cheese) |
| Processed meats (bacon, hot dogs) | Freshly cooked meat, poultry, or fish |
| Red wine | White spirits (in moderation) |
| Citrus fruits | Berries, melon |
| Chocolate | Carob |
| Fermented foods (sauerkraut, kimchi) | Freshly prepared vegetables |
| * Individual responses vary – maintain food diary for tracking | |
Strategic Dietary Management
Only 10% have single-food triggers, but dietary patterns matter. Mediterranean diets show significantly lower attack frequency through omega-3s and polyphenols.
Ketogenic diets help 30% of resistant cases but cause abandonment in 40% due to side effects. Prioritize 5-6 small meals with complex carbs to maintain brain energy without restrictive stress.
Trigger or symptom? The truth about prodrome cravings
Understanding the prodrome phase
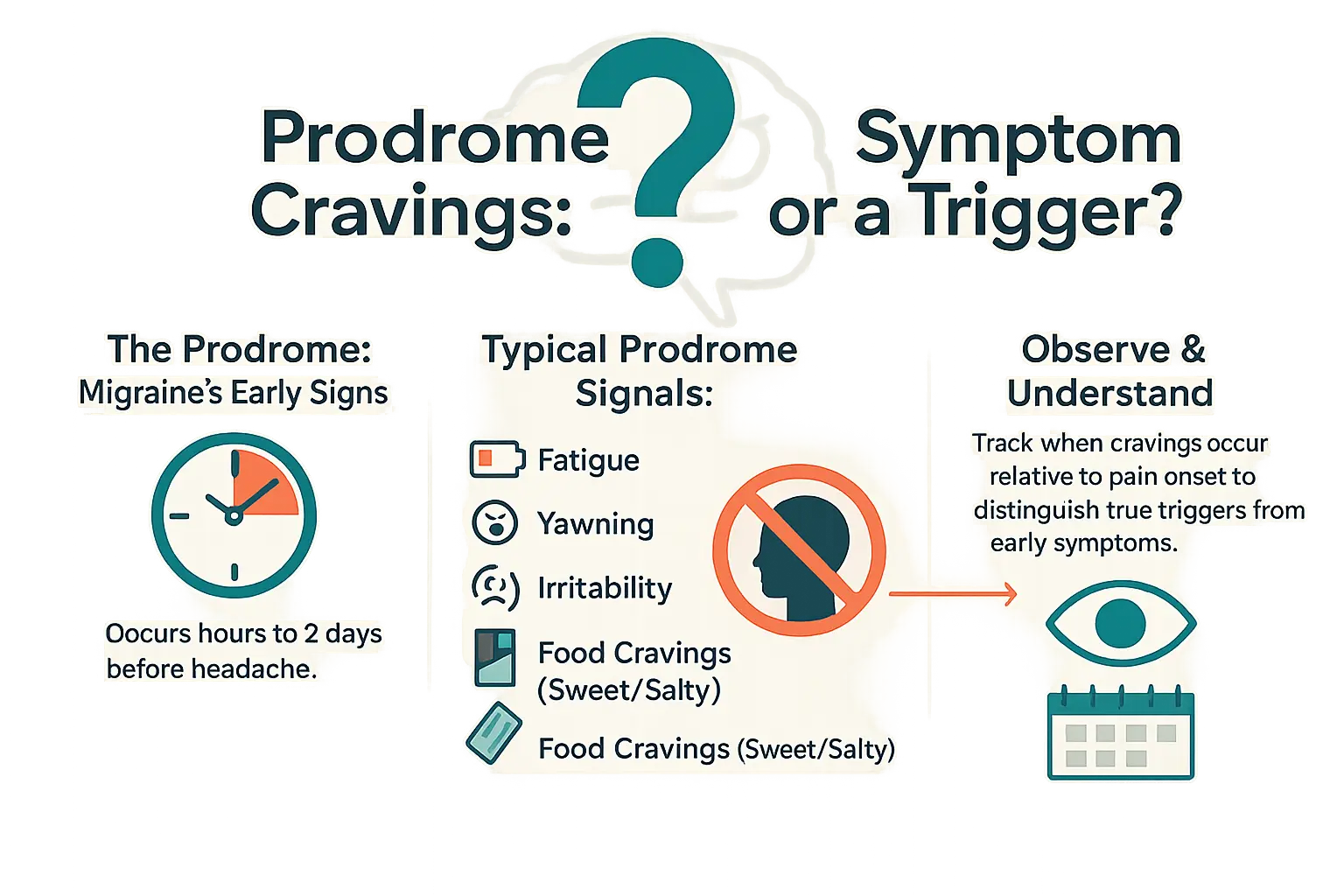
Migraine attacks don’t start with pain. They begin with a prodrome phase lasting hours to two days. This early warning system includes fatigue, neck stiffness, or mood shifts. Recognizing these signs helps you prepare and reduce attack severity. The prodrome phase marks the first stage of a migraine attack, offering a critical window for intervention before pain begins.
Track symptoms like cravings, excessive yawning, or irritability using tools like Migraine Companion to map your patterns. Apps and journals help identify trends over time, turning personal data into actionable insights.
Common prodrome symptoms
Early signs vary but often include:
- Excessive yawning
- Neck pain
- Food cravings (sweet/salty)
- Focus issues
- Thirst changes
- Energy swings
- Urinary frequency or digestion shifts
These aren’t triggers—they’re your brain signaling an approaching attack. Symptoms differ widely between individuals, with about 60% of sufferers experiencing at least one prodrome symptom before each attack.
Chocolate: Trigger or symptom?
Chocolate was long blamed as a migraine trigger. Research shows 61.7% believe it causes attacks, but only 14.3% confirm this personally. Double-blind studies find no difference between chocolate and placebo in triggering headaches. Cravings often appear during prodrome when brain chemistry shifts—your body seeks magnesium or sugar as the attack begins, not causing it. Chocolate contains compounds like flavonoids and magnesium that might actually help prevent attacks when consumed early.
Why timing matters
Log cravings vs. pain onset in a migraine diary. This distinguishes true triggers (weather changes) from prodrome symptoms. Early action—prescribed medication, dark room rest, hydration—can prevent full attacks. Seek medical advice immediately for severe confusion or sudden vision changes.
The hidden factor: How nutritional deficiencies can affect your migraines

Did you know your diet might be making migraines more likely? While specific triggers like stress or weather changes get attention, nutritional deficiencies act like a broken alarm system – creating a lower threshold for migraine triggers.
Brain energy and inflammation
Your brain needs consistent energy and balanced inflammation control. Deficiencies in key nutrients disrupt this balance, increasing migraine vulnerability. inflammation plays a critical role in migraine development.
Magnesium: The calming mineral
This mineral regulates nerve signals and blood vessels in your brain. Low levels increase excitability, making migraines more likely. Found in leafy greens, nuts, whole grains, and dark chocolate, magnesium affects neurotransmitters like serotonin. Studies show many migraine sufferers have lower magnesium levels. However, supplements require medical guidance to avoid interactions.
Riboflavin (B2): Fuel for brain cells
Vitamin B2 fuels mitochondria – brain cell energy centers. Deficiency impairs energy production, increasing migraine vulnerability. Migraine Quebec highlights this link, explaining B2 deficiency increases cellular stress susceptibility. Good sources include dairy, eggs, lean meats, and fortified cereals. Research shows B2 supplementation can reduce migraine frequency.
CoQ10: The energy boost
This antioxidant supports cellular energy production. Low levels correlate with higher migraine frequency. Found in fatty fish, organ meats, whole grains, and nuts, CoQ10 maintains brain cell energy. A 2004 study found 48% of participants taking 100mg CoQ10 thrice daily saw frequency cut in half, compared to 14% with placebo.
Why you shouldn’t self-medicate
“Self-treatment can be dangerous,” warns. Excess magnesium causes digestive issues, while excessive CoQ10 might interfere with blood thinners. Only a doctor can determine deficiencies through testing and recommend safe dosages. Nutritional improvements should complement your migraine management strategy, not replace professional care.
Your best tool: How to identify your personal triggers with a migraine diary
Why track migraines manually when your brain already hurts enough? Berkeley Health reveals a crucial truth: human memory becomes unreliable during neurological crises. A migraine diary isn’t just record-keeping – it’s your personalized detective tool to uncover hidden patterns. This matters because 80% of patients experience “cerebral fog” – a cognitive haze that makes recalling triggers feel impossible.
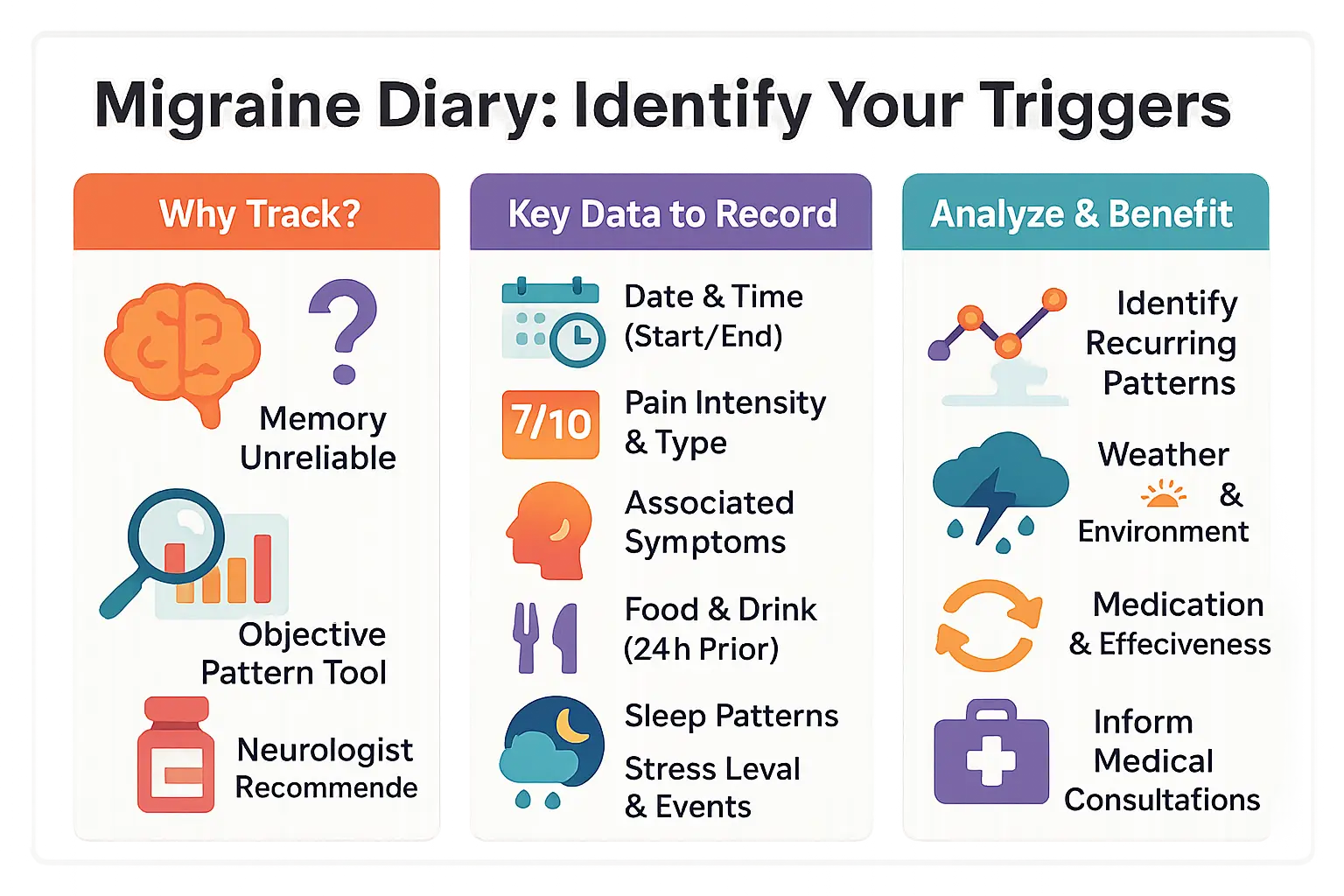
Track these 9 critical elements during each episode:
- Date and time the headache started and ended
- Intensity and type of pain (e.g., 7/10 throbbing pain on one side)
- Associated symptoms (nausea, light sensitivity, aura)
- Food and drink consumed in the preceding 24 hours
- Sleep patterns (quantity and quality of sleep)
- Stress level and specific stress-inducing events
- Menstrual cycle day for women
- Weather changes (temperature, barometric pressure)
- Medication taken and its effectiveness
After 4-6 weeks, look for red flags. Does inadequate sleep combined with wine consumption consistently precede attacks? Does weather shift correlate with specific symptom patterns? This isn’t just data collection – it’s building your personal migraine map. La Voix des Migraineux emphasizes how these patterns transform patient-doctor conversations from vague descriptions to actionable insights. Every entry fills the gaps between clinical visits, creating a timeline that might reveal surprising connections – like how skipping breakfast on stressful mornings doubles your attack risk. Remember, 65% of hormonal migraine sufferers discover their patterns through consistent tracking, while 53% of weather-sensitive patients adjust their routines once patterns emerge.
From Identification to Action: Creating Your Trigger Management Strategy
Why Knowing Your Triggers Empowers You
Migraines aren’t one-size-fits-all. Triggers like stress, weather shifts, or foods vary individually. Tracking patterns reduces attacks by 40% (Migraine Quebec). The aim isn’t to fear triggers but to create a personalized strategy that fits your life.
Focus on the Big Rocks First
Prioritize high-impact habits: sleep, stress, and diet. Irregular rest increases sensitivity—aim for 7-9 hours nightly. For stress, mindfulness or controlled breathing (La Voix des Migraineux recommends 4-4-8 breathing) lowers cortisol spikes. Limit processed foods and stay hydrated—simple steps reduce overall vulnerability.
Build a Proactive Lifestyle
Managing triggers means building resilience. Activities like walking or yoga boost well-being. For tailored support, improve your daily life with routines stabilizing your nervous system. They’re part of your journey, not your identity. Small, consistent actions create lasting change.
FAQ
What are the 5 C’s of migraines?
While there’s no official “5 C’s” list for migraines, common triggers often start with these categories: Caffeine (both excess and withdrawal), Cheese (aged varieties like cheddar), Chocolate (though it may be a prodrome symptom, not a direct trigger), Citrus fruits, and Climate changes (like weather shifts). These vary individually, so tracking your personal patterns is key. For example, a 2023 study found nearly 100% of migraineurs had multiple triggers, emphasizing their personalized nature.
What are the main triggers for migraines?
Migraine triggers fall into five broad categories: 1. Stress (emotional or physical, including post-stress relaxation). 2. Sleep issues (too little or too much sleep). 3. Hormonal shifts (like estrogen fluctuations in women). 4. Environmental factors (weather changes, bright lights, loud sounds). 5. Dietary elements (alcohol, aged cheeses, processed meats, and irregular eating). Each person’s brain has a unique “migraine threshold,” so triggers often combine (e.g., a sleepless night + stress + weather change) to push past that tipping point.
How do I stop getting so many migraines?
Start by identifying your personal triggers through a migraine diary, tracking diet, sleep, stress, and weather. Focus on lifestyle adjustments: – Keep consistent sleep and meal times. – Manage stress with meditation or yoga. – Stay hydrated and limit known dietary triggers. For frequent attacks, consult a neurologist. Preventive treatments like beta-blockers or CGRP inhibitors might be recommended. Remember, the goal isn’t perfection but reducing frequency—stabilizing “big rocks” like sleep and stress often lowers sensitivity to smaller triggers.
How does amitriptyline work for migraines?
Amitriptyline, a tricyclic antidepressant, helps prevent migraines by regulating brain chemicals like serotonin and norepinephrine. It’s used “off-label” for migraine prevention, meaning it’s not FDA-approved but widely prescribed. Studies suggest it lowers attack frequency by stabilizing nerve pathways. Side effects (drowsiness, dry mouth) are common, so doctors may start with low doses. Always consult a specialist before starting—this medication requires careful management.
How to get rid of a migraine fast?
Act quickly with: – Medications: Over-the-counter NSAIDs (ibuprofen) or triptans (sumatriptan) for moderate/severe attacks. – Hydration: Sip water—dehydration worsens symptoms. – Environment: Rest in a dark, quiet room. – Cold therapy: Apply a cool compress to your forehead. If pain persists, seek medical advice. For chronic migraines, discuss preventive strategies with your doctor to reduce future episodes.
What do migraines do to the brain?
Migraines involve complex brain activity: – The trigeminal nerve activates, releasing inflammatory substances that sensitize pain pathways. – Serotonin levels drop, affecting pain regulation. – CGRP (calcitonin gene-related peptide) surges, causing blood vessel dilation and inflammation. These processes explain symptoms like light sensitivity and aura. Over time, frequent migraines may alter brain structure, but early management (preventives, trigger avoidance) can reduce long-term impacts.
Why am I getting migraines all of a sudden?
Sudden migraines often stem from a “trigger stack”—multiple factors combining to breach your threshold. For example: – A stressful week + poor sleep + hormonal changes – Dehydration + bright sunlight + skipped meals New triggers (e.g., a job change) can also emerge. Track patterns in your diary and consult a doctor if attacks increase—new preventive treatments or lifestyle shifts might be needed.
What is the permanent cure for migraine?
There’s no permanent cure, but migraines can be managed: – Lifestyle tweaks (regular routines, stress reduction). – Preventive meds (amitriptyline, CGRP inhibitors). – Acute treatments (triptans, gepants). Research explores nerve-stimulation devices and gene therapy, but current care focuses on minimizing disruptions. Work with your doctor to create a tailored plan that balances prevention and acute care.
What are you lacking if you get migraines?
Some studies link deficiencies to migraines, though causality isn’t proven: – Magnesium: Involved in nerve function; low levels might increase brain excitability. – Vitamin B2 (Riboflavin): Supports brain energy production. – CoQ10: An antioxidant that aids cellular energy. Supplements may help some, but consult your doctor first—excess magnesium can cause diarrhea, and CoQ10’s safety in pregnancy isn’t established. Focus on a balanced diet rich in leafy greens, nuts, and lean proteins before supplementing.