Are you struggling to tell if that crushing pressure is just a common stress reaction or a severe migraine tension headache that forces you into a dark, silent room? Recognizing these distinct pains is your primary weapon for ending the frustrating guesswork and finally choosing a medical treatment path that restores your daily freedom and mental clarity. Our guide provides the roadmap to identify your specific triggers and master the proven relief strategies that effectively stop these invisible attackers before they steal your professional productivity or ruin your precious family time forever.
Deciphering Head Pain: Migraine vs. Tension Headache
You are likely staring at the ceiling, wondering if your head is trapped in a literal vice or if a neurological storm is brewing. Distinguishing between these two types of pain is your first real move toward finding lasting relief and reclaiming your day.
Defining the Two Primary Headache Types
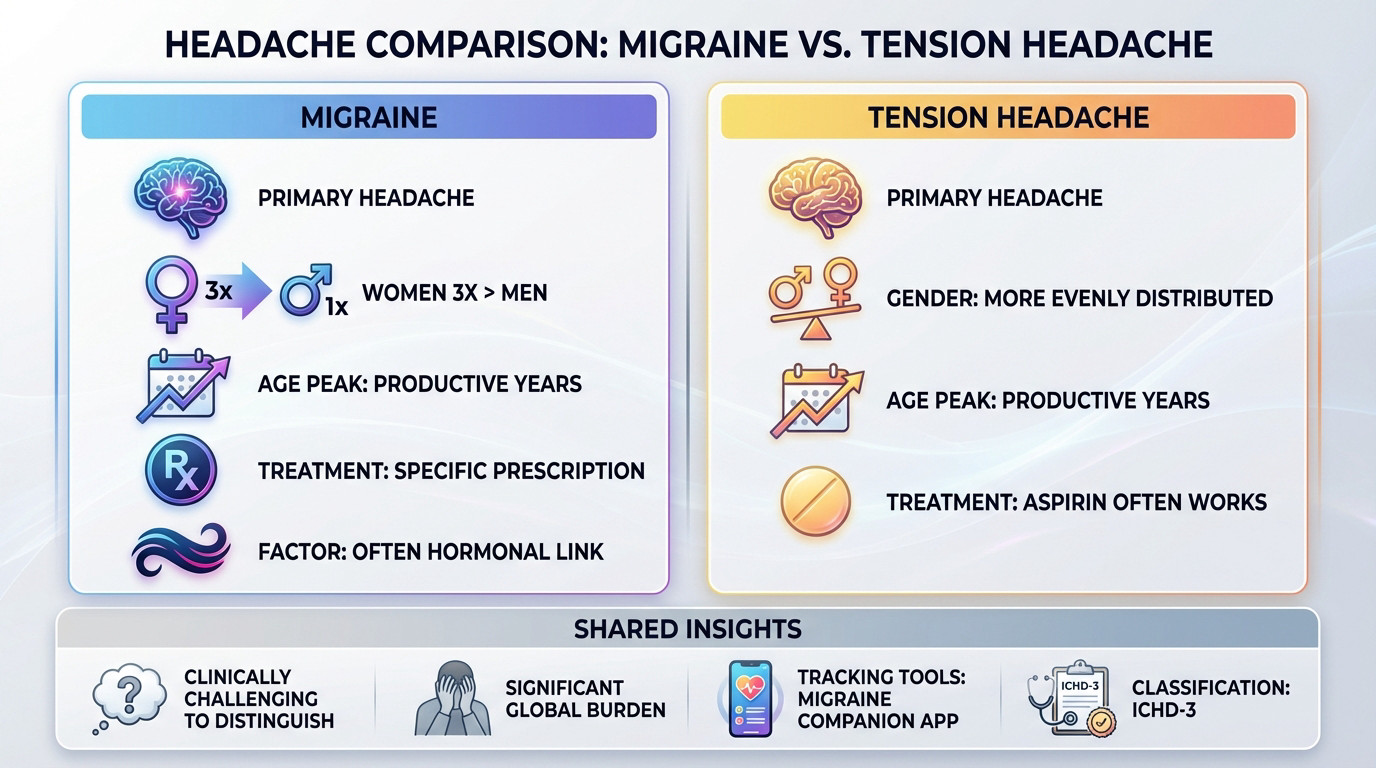
Tension headaches and migraines are both primary headaches. They share a label but have distinct neurological roots. Their impact on your life varies wildly. Doctors often find them tricky to tell apart.
These conditions affect millions globally every day. Research using the ICHD-3 classification highlights their massive reach. Most adults will face one eventually.
Getting the diagnosis right changes your treatment. You might need simple aspirin or a specific prescription. Using the Migraine Companion app helps track these differences clearly.
Prevalence and Demographic Trends
Gender plays a massive role here. Migraines hit women three times more often, usually linked to hormones. Tension headaches are fairer, affecting everyone more equally.
Most people suffer during their peak productive years. This creates a heavy burden on work and family. It is a global struggle for millions.
Hormones often dictate the frequency of attacks. You can learn more about migraines and menstrual cycle patterns. This link explains much of the female prevalence.
Symptom Comparison: Spotting the Differences
Move from the general definitions to the specific physical sensations.
Pain Location and Quality
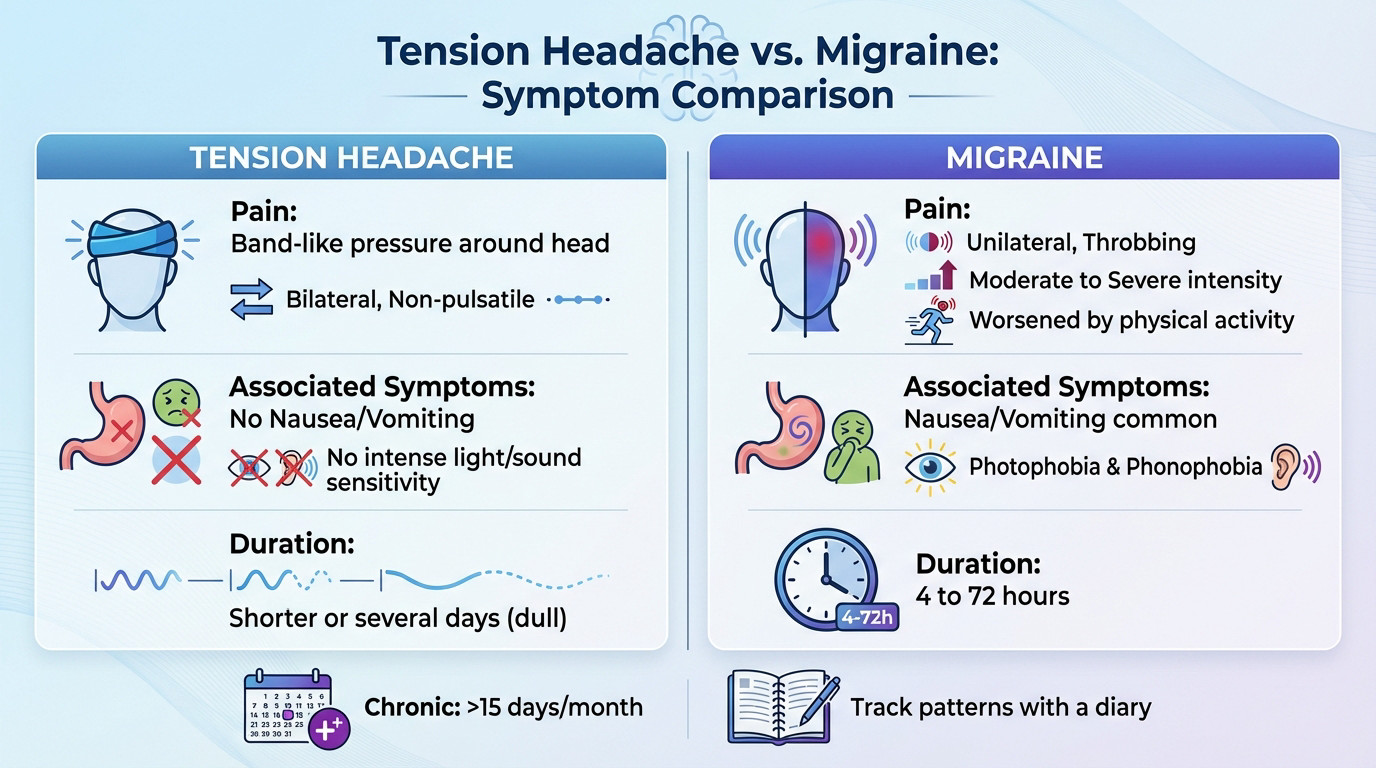
Tension pain acts like a tight band squeezing your skull. It stays bilateral and non-pulsatile. Experts at MedlinePlus identify this as the most frequent headache type.
Migraine pain feels drastically different, usually unilateral and throbbing. The intensity is moderate to severe. Physical activity often makes the pain much worse. This movement-triggered agony rarely happens with simple tension headaches.
Explore what is a migraine to see the deep neurological side. Knowing the difference stops the guesswork and starts the healing.
Associated Neurological Symptoms
Focus on nausea and vomiting. These are hallmark migraine symptoms almost never present in tension-type headaches. This serves as a primary diagnostic clue for many.
Sensory sensitivity is another massive factor. Migraineurs often hide in dark, quiet rooms. Photophobia and phonophobia are intense during attacks. The WHO criteria confirm these sensitivities define the condition’s severity.
Tension headaches lack these intense neurological features. They might be annoying or distracting. But they rarely force you into total isolation or a pitch-black room for days.
Duration and Frequency Patterns
Compare the “attack” duration. Migraines typically last 4 to 72 hours. Tension headaches can be shorter or linger for several days in a dull, constant state.
Understand chronic vs. episodic patterns. If pain occurs more than 15 days a month, it is considered chronic. This situation requires a much more aggressive management strategy.
Use the Migraine Companion diary to track these durations. Patterns often reveal the true nature of the headache.
References
- MedlinePlus: Tension Headache Information
- World Health Organization (WHO): Headache Disorders Fact Sheet
The Role of Aura and Premonitory Phases
You might think the pain is the whole story. But for many, that throbbing headache is just one chapter in a much longer neurological event. This timeline is the real key to the riddle: Tension headache vs migraine – how to know?
Understanding the Migraine Aura
The aura acts as a strange warning signal. It involves visual or sensory disturbances that flare up. You might see flashing lights or feel tingling in your hands. These signs usually arrive before the actual pain hits.
Statistics show only 20% of sufferers experience these neurological warning signs. It remains a distinct marker of the condition. Most people never see these visual sparks at all.
Explore the various types of migraines to see where aura fits. This particular subtype requires unique management. Recognizing it early helps you take control faster.
The Prodrome and Postdrome Phases
The prodrome starts days before the attack. Symptoms like yawning or neck stiffness appear early. These signals are unique to migraines and absent in tension headaches.
Then comes the “migraine hangover” or postdrome phase. Once the pain fades, you feel completely drained or confused. This recovery can last 24 hours. It highlights the systemic nature of this neurological disease.
Contrast this with a typical tension headache. Once that pressure lifts, you usually feel normal again immediately. There is no lingering neurological fog or deep exhaustion.
Triggers and Causes: What Sets Them Off?
Differentiating between these pains is vital. When looking at Tension headache vs migraine: how to know? It starts by identifying the specific catalysts involved.
Stress and Physical Strain
Stress is a universal thief of comfort. It forces your neck muscles into a tight knot. This constant contraction is the primary driver for most nagging tension-type headaches you face.
You are not alone in this fight. Explore this stress migraine link explaining why 80% of attacks are triggered by it. High tension levels often turn minor pressure into a crisis.
Your desk setup might be the enemy. Slouching over a laptop for hours creates immense physical strain. These office headaches are usually tension-based, born from poor ergonomics and stiff shoulders.
Environmental and Lifestyle Triggers
Migraines thrive on sensory chaos. Skipped meals, harsh lights, and pungent smells act as instant fuses. For sensitive brains, even a sudden shift in the wind can spark an episode.
Watch the skies closely. Many sufferers feel storms in their temples. Check the science of barometric pressure migraines to see how atmospheric drops irritate nerves and trigger inflammation.
Tension headaches usually ignore the weather. They care about your muscle state. Unlike migraines, they rarely flare up just because the sun is too bright.
The Role of Sleep and Diet
Sleep is a delicate balance for your brain. Both oversleeping and exhaustion can trigger pain. Consistency is your best defense, keeping your neurological system stable and much less reactive.
Aged cheeses and nitrates are common dietary villains. While controversial, many find specific foods problematic. Tracking diet in the Migraine Companion app helps you identify these personal triggers effectively.
Morning pain often has roots in your rest patterns. Read about night morning migraines to understand why your sleeping habits are the foundation of a pain-free life.
References
Treatment and Relief Strategies
Now that we know what they are and why they happen, let’s look at how to stop the pain.
Over-The-Counter and Prescription Options
You reach for the medicine cabinet when the pressure hits. Determining a tension headache vs migraine – how to know? starts with the right treatment. Ibuprofen or acetaminophen work well for tension. They also help mild migraines.
Triptans are migraine-specific medications targeting the trigeminovascular system. They do not work for tension headaches. This remains a key distinction for your diagnosis. You need the right tool for the job.
Watch out for rebound pain. Taking pills too often creates medication overuse headaches. This makes your original condition much harder to treat. You end up in a cycle of suffering.
Non-Pharmacological Approaches
Pills aren’t the only answer available to you. Biofeedback and acupuncture can effectively reduce tension. Neck-strengthening exercises work wonders for chronic tension-type headaches. These are helpful if poor posture or physical strain causes your pain.
You can also explore migraine relief tips for home remedies like deep breathing. These techniques calm your nervous system. They offer natural pressure management without side effects.
Stay hydrated and eat regular meals. These habits stabilize your internal environment. They prevent the sudden “dips” that often lead to a migraine. Consistency is your best defense.
When to See a Doctor
Identify red flags immediately. Seek help if you have a “thunderclap” headache. Also, see a professional if your headache pattern changes suddenly. Never ignore these shifts in your health.
A diagnosis provides clarity. Doctors rule out serious issues. They also offer access to newer treatments like CGRP inhibitors for chronic pain. You deserve an expert partner in your care.
Bring your Migraine Companion data to the appointment. It provides the doctor with objective evidence of your symptoms. This makes your consultation more productive.
References
Check the scientific sources used to verify the accuracy of this guide on tension headache vs migraine: how to know?
Scientific Sources and Clinical Guidelines
We rely on the Journal of Headache and Pain for precise data. MedlinePlus offers the clinical definitions used throughout this guide. These authorities provide the foundation for our medical insights.
The World Health Organization and UC Berkeley provided key statistics. Their research supports our sections on prevalence and specific symptoms.
All links are provided in the text. Consult them for deeper clinical details.
Differentiating your migraine tension headache symptoms depends on spotting either a tight band sensation or throbbing pain with nausea. Start logging your symptoms today to secure the precise treatment you deserve. Reclaim your comfort and embrace a future where you are finally in control of your health.
FAQ
How can you tell the difference between a migraine and a tension headache?
Differentiating the two is the first step toward reclaiming your day. A tension headache typically feels like a tight band squeezing both sides of your head with a dull, steady ache. It is distracting but rarely stops you from finishing your tasks.
Migraines are far more intense and neurological in nature. They usually cause a throbbing or pulsing sensation, often on just one side of the head. Unlike tension headaches, migraines frequently bring nausea, vomiting, and extreme sensitivity to light or sound.
What are the hallmark symptoms of a tension-type headache?
You will likely feel a sensation of pressure or tightness across your forehead, temples, or the back of your head. Many describe it as having their head held in a tightening vice. This pain is usually mild to moderate and does not get worse with physical activity.
You might also notice muscle tenderness in your scalp, neck, and shoulders. Crucially, tension headaches do not cause the visual disturbances or stomach upset that define the migraine experience.
What is a migraine aura and do tension headaches have them?
An aura is a specific neurological event that occurs only with migraines, never with tension headaches. You might see flashing lights, wavy lines, or experience temporary blind spots. Some people also feel tingling in their arms or face shortly before the pain begins.
Only about 20% of migraine sufferers experience this phase. It serves as a clear warning sign that a migraine attack is imminent. If you experience these sensory changes, you are dealing with a migraine, not a regular headache.
How long does the pain typically last for each headache type?
Timing is a key clue for your diagnosis. A tension headache is highly variable; it can last as little as 30 minutes or linger as a dull ache for several days. They often worsen as the day progresses but rarely wake you from sleep.
Migraine attacks are generally more structured, typically lasting between 4 and 72 hours. If your pain lasts longer than three days without relief, it is classified as status migrainosus and requires professional medical attention.
What are the most common triggers for these headaches?
Stress is the universal enemy for both types. For tension headaches, physical strain from poor posture or clenching your jaw often sets off the pain. It is the classic “office headache” caused by hours at a computer.
Migraines have a much wider range of triggers. You might be sensitive to hormonal shifts, weather changes, or skipped meals. Identifying these patterns in a diary is essential for we to help you find the right prevention strategy.
When is it time to stop self-treating and see a doctor?
You should seek medical advice if your headaches become more frequent or if the pattern of pain suddenly changes. If you are relying on over-the-counter pills more than twice a week, you risk developing “rebound” headaches that make the condition worse.
Immediate medical care is necessary if you experience a “thunderclap” headache, fever, a stiff neck, or sudden confusion. These red flags require an urgent professional evaluation to rule out serious underlying issues.