If you often feel the world tilt or the floor drop away without a headache, recognizing vestibular migraine symptoms is the first step toward reclaiming your sense of balance. This disorienting experience affects thousands of us, yet it remains frequently misunderstood because it mimics other inner ear disorders or presents as a silent neurological storm. By exploring the science behind these dizzy spells and learning to track your personal triggers, you can finally gain the clarity needed to manage your health and stop feeling like you are constantly walking on a moving ship.
Understanding Vestibular Migraine Symptoms and What They Feel Like
Migraine is more than a headache; it is a sensory storm that throws your whole world off balance.
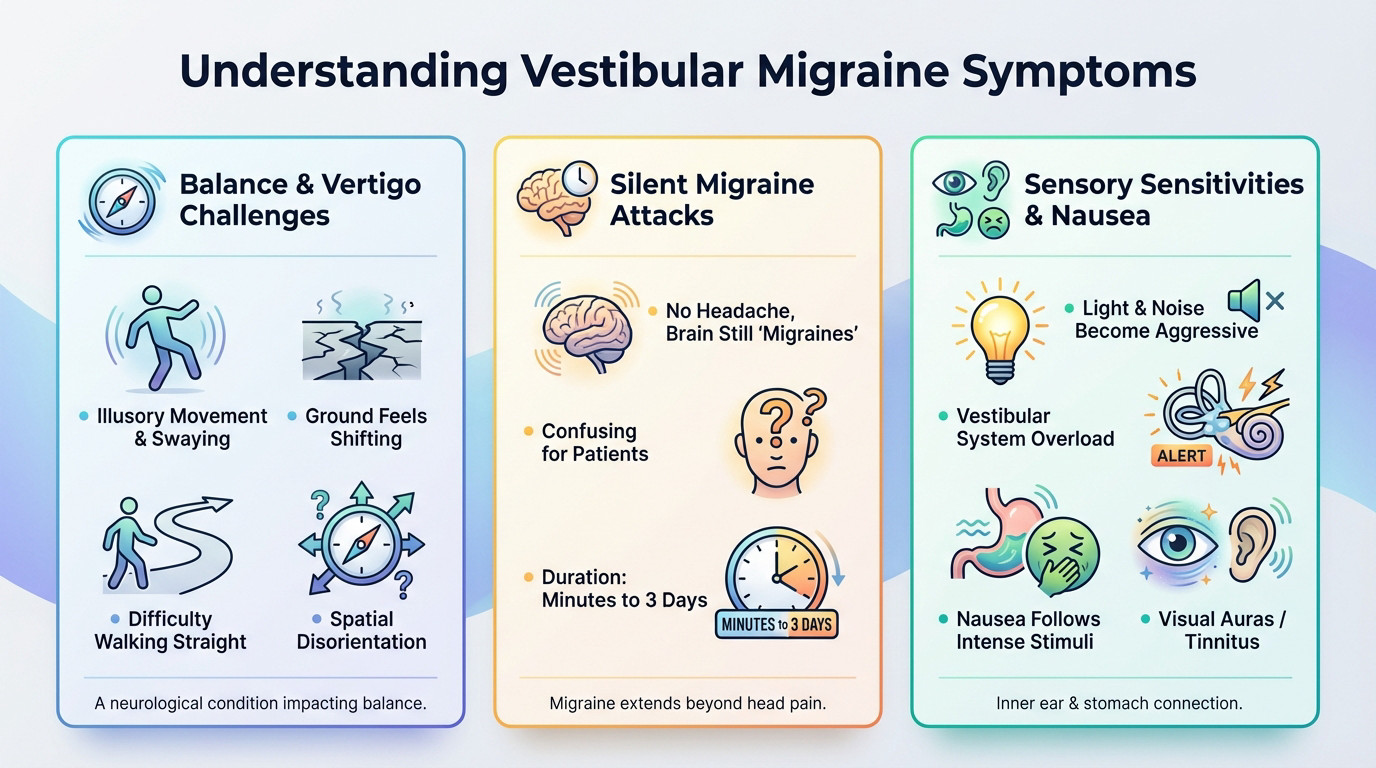
The Reality of Vertigo and Internal Balance Issues
You might feel the floor dropping away. It is not just spinning; it feels like rocking on a boat. Your brain creates false motion.
Walking straight becomes a struggle. This spatial disorientation makes simple trips to the store feel totally overwhelming.
This vestibular migraine study shows it is a neurological condition disrupting balance.
Why You Might Feel Dizzy Without a Headache
Many patients experience a silent migraine. No head pain is involved. Instead, the brain processes signals through dizziness and persistent vertigo.
Episodes can last five minutes or stretch into three days. Time feels elastic.
Understanding what is a migraine clarifies that pain is optional.
Associated Sensory Sensitivities and Nausea
Bright lights and loud noises feel like attacks. Your vestibular system cannot cope. Nausea follows these intense stimuli.
You might see flickering spots or hear ringing. These auras and tinnitus often signal an attack.
The inner ear and stomach are linked. This duo makes dizzy spells nauseating.
References
Common Triggers and the Science Behind the Dizzy Spells
After describing the vestibular migraine symptoms you feel, it is time to understand why your brain decides to make you tilt without warning.
Hormones and Stress as Primary Biological Drivers
Hormones act as biological heavy hitters. The menstrual cycle frequently stirs up these vestibular storms. Serotonin simply fails to regulate balance and pain signals correctly.
Stress stands as the ultimate trigger. One sharp anxiety spike and vertigo settles in. It is a draining cycle.
Learn about this stress migraine link now. It explains so much.
Environmental Factors and Food-Related Sensitivities
The weather is rarely an innocent bystander. Rapid barometric pressure drops often kickstart the spinning. Inflammatory foods also aggravate your sensitive nervous system.
Monitor barometric pressure migraines during seasonal shifts. It makes a huge difference.
Many sufferers dealt with car sickness during childhood. That motion sensitivity usually lingers.
Tracking Patterns with Migraine Companion
A tracking app truly shifts the perspective. Recording episodes uncovers hidden patterns in your life. You eventually see what causes the break.
Calendars help link weather to your diet. This data offers real proof for your medical team. It provides much-needed control.
Try the Migraine Companion app to find your patterns. Identify your personal triggers easily.
How Do Doctors Distinguish Migraine From Other Ear Disorders?
Identifying the culprit isn’t simple, as the inner ear hides its secrets behind overlapping symptoms.
Comparing Symptoms with Meniere Disease and BPPV
Meniere’s disease usually triggers permanent hearing loss over time. But BPPV involves displaced ear crystals. Vestibular migraine symptoms often leave physical exams looking remarkably “clean.” An MRI frequently shows nothing, which feels incredibly frustrating for us.
Doctors track nystagmus, those involuntary eye flickers. This helps them rule out mechanical ear failures. Ultimately, the diagnosis remains clinical, relying on your specific history and patterns.
Check this study to distinguish vestibular migraine from Meniere. It clarifies the confusion.
Meeting the ICHD-3 Criteria for a Formal Diagnosis
You need five distinct episodes to validate the diagnosis. These ICHD-3 rules are quite rigid. Your history of classical migraines carries significant weight during these medical talks.
Specialists follow diagnostic criteria from the International Bárány Society. These guidelines help when tracking your migraine patterns. They make sure doctors don’t overlook subtle vestibular signs.
This elimination process takes time. We rule out serious neurological threats before settling on a conclusion through a path of true patience.
3 Effective Strategies to Manage and Prevent Future Attacks
Once the diagnosis is confirmed, the goal is clear: regaining control and refusing to let every pressure change dictate your life.
Preventive and Abortive Medical Options for Stability
Beta-blockers help stabilize your system effectively. Anti-epileptic drugs often provide another frequent clinical option. These background treatments aim to reduce how often your painful attacks actually occur.
Rescue treatments exist especially for acute episodes. They stop the spinning sensation before it fully takes hold. You must act fast as soon as those first warning signs appear.
Supplements like magnesium prove quite useful. Riboflavin also helps a lot. These natural choices support your nervous system’s health.
Check out these migraine relief tips for more help. They really make a difference.
Physical Therapy and Lifestyle Hygiene for Long-Term Relief
Vestibular rehabilitation is a secret weapon. It teaches the brain to ignore those confusing, false signals. Think of it as gymnastics for your balance. The long-term results are often quite impressive for many of us.
Lifestyle hygiene is absolutely non-negotiable. Stick to fixed sleep times. Hydrate yourself without waiting for thirst. These simple habits protect your sensitive brain from sudden sensory overloads.
Stress management through mindfulness really works. Learning to breathe calms your nervous system. It is free and remarkably effective for daily life.
Recognizing vestibular migraine symptoms and distinguishing them from other ear disorders is your first step toward reclaiming steady ground. By tracking your patterns today, you can work with specialists to build a life where balance is the norm. You deserve a future where dizziness no longer dictates your daily rhythm.
FAQ
What exactly does a vestibular migraine feel like?
A vestibular migraine is a complex neurological event that primarily affects your sense of balance rather than just causing pain. You might experience spontaneous vertigo (a spinning sensation), a feeling of rocking as if you are on a boat, or a deep sense of spatial disorientation. Many of us also deal with nausea, sensitivity to light (photophobia), and sound (phonophobie), along with ear-related symptoms like tinnitus or a feeling of fullness in the ear.
These episodes are quite variable; they can last from a few minutes to several days. It is important to know that these sensations are real and result from your brain misinterpreting balance signals, often making everyday activities like walking or driving feel overwhelming.
Is it possible to have a vestibular migraine without a headache?
Yes, it is very common. This is often referred to as a “silent migraine” or acephalgic migraine. In these instances, you may not feel any throbbing head pain at all, but you still experience the intense dizziness, motion sensitivity, or visual auras associated with a migraine attack. This can be quite confusing for those newly diagnosed, as we often think a migraine must involve a severe headache.
How do doctors distinguish vestibular migraine from Meniere’s disease or BPPV?
Doctors look closely at the timing and nature of your symptoms to tell these apart. BPPV (Benign Paroxysmal Positional Vertigo) usually causes very brief bursts of spinning, lasting only seconds, triggered by specific head movements. Meniere’s disease is typically characterized by progressive hearing loss and longer episodes of vertigo. Vestibular migraine is often identified by a personal history of migraines and the fact that symptoms often respond well to migraine-specific lifestyle changes or treatments.
What are the official diagnostic criteria for vestibular migraine?
According to the ICHD-3 and the Bárány Society, a formal diagnosis requires at least five episodes of moderate to severe vestibular symptoms lasting between 5 minutes and 72 hours. Furthermore, you must have a current or past history of migraines. Finally, at least half of your dizzy spells must be accompanied by at least one migraine feature, such as a pulsating headache, light and sound sensitivity, or a visual aura.
What are the most common triggers for these dizzy spells?
Triggers vary from person to person, but common culprits include hormonal shifts (like the menstrual cycle), high levels of stress, and lack of sleep. Environmental factors like changes in barometric pressure or bright, flickering lights can also set off an attack. Some people also notice that certain inflammatory foods or dehydration can make their system more vulnerable to a vestibular episode.
How can I manage or prevent future vestibular migraine attacks?
Management usually involves a combination of medical and lifestyle strategies. Doctors may prescribe preventive medications like beta-blockers or anti-seizure drugs to stabilize the nervous system. Vestibular rehabilitation therapy is also a fantastic tool; it’s a form of physical therapy that helps “retrain” your brain to handle balance signals correctly.
On a daily basis, maintaining a regular sleep routine and staying hydrated are essential. Many in our community find it incredibly helpful to use the Migraine Companion app to track their symptoms. By logging your attacks, you can identify patterns—like weather changes or specific foods—that might be triggering your dizziness, allowing you to take proactive steps toward relief.