Does that relentless pressure behind your eyes feel like an endless infection, yet every decongestant fails to bring the relief you deserve when battling a sinus headache migraine? Understanding the true source of this throbbing, invisible weight is the first step toward reclaiming your life from a nervous system that mimics congestion to trick your senses. Our guide exposes the surprising truth about these neurological illusions, revealing specific signs like nausea or light sensitivity that finally clarify your diagnosis, stop the cycle of ineffective treatments, and start a path toward real, lasting comfort today.
The Myth of the Sinus Headache: Why 90% Are Actually Migraines
You might ask: Migraine or sinus headache? How to tell the difference, even if it feels like both sides of the face are exploding? Your face isn’t infected; your brain is simply sounding a false alarm.
The Surprising Statistics of Misdiagnosis
Studies confirm that 90% of self-diagnosed sinus headaches are actually migraines. This confusion is widespread and persistent. Most patients mistake neurological signals for infection. It remains a massive diagnostic blind spot.
General practitioners often fall into this trap. This error represents a significant and growing public health challenge.
Misdiagnosis results in ineffective care. Antibiotics won’t help because they cannot treat a hyper-reactive migraine brain.
Why Your Brain Mimics a Sinus Infection
The trigeminal nerve is the culprit. It carries pain signals to your face during migraine attacks. This creates the false sensation of sinus pressure.
Your autonomic nervous system also reacts. It causes nasal congestion or tearing eyes, perfectly mimicking a sinus infection.
The symptoms are misleading. You suspect bacteria, but the cause is entirely neurological.
Spotting the Difference: Key Symptoms to Watch For
Now that we understand why the confusion exists, let’s look at how to concretely differentiate these two states so you stop reaching for the wrong remedy.
The Triple Threat: Nausea, Light, and Sound
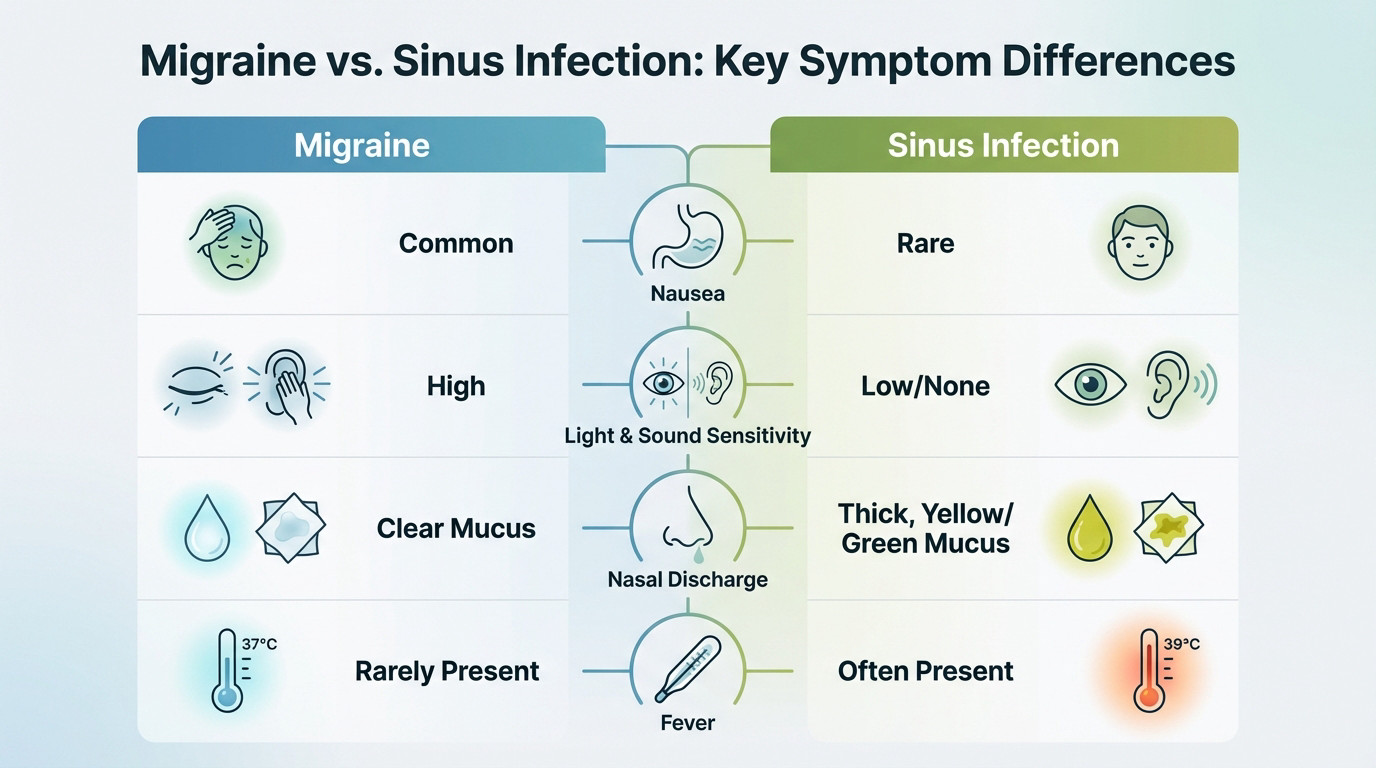
Feeling sick to your stomach? If nausea hits, it’s almost certainly a migraine. Sinus infections rarely cause that queasy feeling, making this a reliable indicator for your self-diagnosis.
Sensitivity to light and noise is another major red flag. Migraine sufferers often retreat into total darkness. Sinusitis simply doesn’t demand that kind of sensory isolation.
These signs form the heart of your diagnosis. You can find more help distinguishing between a migraine and a standard headache here. Don’t ignore these specific neurological clues.
Clear vs Discolored Nasal Discharge
Check your tissue immediately. Clear mucus often accompanies migraines due to autonomic system activation. Thick, yellow, or green discharge signals a real infection. This distinction is absolutely fundamental for your recovery path and future treatment.
Fever acts as a definitive marker for infection. It almost never appears during a standard migraine attack.
Without infection signs, seek a neurological cause. Stop using useless nasal sprays that won’t help.
Triggers and Patterns: The Environmental Connection
Beyond the physical symptoms, timing and environment offer the most revealing clues about your pain’s true origin.
The Weather and Barometric Pressure Trap
Weather shifts affect both conditions. Pressure swells sinus tissues. Yet, for a Migraine or sinus headache? How to tell the difference, both sides of the face, weather triggers migraines.
Your brain is hypersensitive to atmospheric pressure changes. This specific variation is an ultra-frequent trigger. It disrupts fluid balance in nasal tissues. This often mimics a sinus infection perfectly.
Don’t assume humidity alone infects your sinuses. It might simply irritate your highly sensitive nervous system instead.
Tracking Your Attacks for Clarity
A migraine follows a cyclical pattern. Sinusitis usually persists longer without any break. Record your attack frequency to identify the underlying rhythm.
Use the Migraine Companion app to monitor these episodes. This reveals if your “sinus issues” recur monthly. Download it here: Migraine Companion.
Hard data never lies. It helps your doctor provide an accurate diagnosis much faster.
Effective Relief: Moving Beyond Antibiotics
Once your diagnosis is clear, it’s time to swap your pharmacy shelf to target the real source of that facial agony.
Why Triptans Work When Decongestants Fail
If a triptan stops your pain, it’s proof. These drugs target migraines, not bacteria. It is a diagnostic test. See Harvard Health: Migraine or sinus headache? How to tell the difference ,both%20sides%20of%20the%20face.
Decongestants might offer a temporary placebo boost. But they never treat the underlying neurological cause. Your facial pain will return quickly.
Shift your strategy now. Target the nervous system, not just your nose.
When to Seek Professional Help
Seek help if the pain becomes unbearable. A neurologist often provides more clarity than an ENT. Don’t let migraines become a chronic, daily burden.
Watch for emergency signs like confusion or sudden weakness. Safety always comes first. Learn to recognize these serious red flags immediately and act.
A proper diagnosis changes everything. Stop living in doubt. Start healing.
Stop guessing: 90% of facial pressure is actually a migraine, not an infection. Track your symptoms now to accurately identify your sinus headache migraine and access the treatment you truly need. Reclaiming your pain-free life starts with the right diagnosis today.
FAQ
How can I truly tell the difference between a migraine and a sinus headache?
It is incredibly common to mistake one for the other, but the key lies in your specific symptoms. While both cause facial pressure, a migraine is almost always accompanied by nausea or sensitivity to light and sound. If you feel the urge to lie down in a dark, quiet room, you are likely experiencing a neurological event rather than an infection.
True sinus headaches, or rhinosinusitis, are actually quite rare and usually follow a cold. They are defined by a fever and thick, discolored mucus. Without these signs of infection, there is a 90% chance that your “sinus” pain is clinically a migraine. Identifying these differences is the first step toward getting the relief you deserve.
Does the color of my mucus indicate an infection or a migraine?
Your tissue provides a vital clue. Clear, thin drainage is common during migraines because the autonomic nervous system can become overactive, causing your nose to run. However, if your mucus is thick, yellow, or green, your body is likely fighting a viral or bacterial infection. This discoloration is a primary hallmark of actual sinusitis.
Do not let clear drainage trick you into taking unnecessary antibiotics. If your “sinus” symptoms appear without a fever or colored discharge, your brain—not an infection—is the likely culprit. Recognizing this distinction prevents you from using ineffective treatments that fail to stop the pain.
Why do I feel so much pressure in my face if it is actually a migraine?
This confusion happens because of the trigeminal nerve. This nerve is responsible for carrying pain signals from your face, eyes, and jaw directly to your brain. During a migraine, this nerve becomes highly irritated, creating a powerful illusion of pressure and fullness behind your cheeks and forehead, even when your sinuses are completely clear.
This neurological “trick” is why many people reach for decongestants that offer no real help. Your face feels heavy, but the root cause is a sensitive nervous system. Understanding this connection helps you move past the myth of the sinus headache and toward a strategy that actually works.
Can weather changes trigger both sinus pain and migraine attacks?
Yes, but the way your body reacts depends on your sensitivity. Shifts in barometric pressure can cause the tissues in your sinuses to swell, but they are also a major trigger for the hypersensitive migraine brain. Many people assume a passing storm means a “sinus” issue, when it is actually their nervous system reacting to the environmental shift.
If your headaches follow a pattern with the weather, tracking them can provide much-needed clarity. Using an tool like the Migraine Companion app allows you to see if these “sinus” episodes are actually cyclical. This data helps your doctor provide a faster, more accurate diagnosis so you can stop guessing.
When should I seek professional medical help for my facial pain?
You should consult a professional if your headaches occur more than 15 days a month or if over-the-counter medications no longer provide relief. If you experience red flags like a sudden “worst headache ever,” confusion, or high fever with extreme facial tenderness, seek immediate care. A neurologist can often provide the specific migraine treatments that an ENT cannot.
Don’t wait for the pain to become chronic or life-altering. If your “sinus” issues keep returning month after month, it is time to investigate the neurological side of your health. A proper diagnosis changes everything, allowing you to reclaim your life from the cycle of pain.