That intense, throbbing pain that makes you retreat to a dark, quiet room—is it just a bad headache, or something more complex? The migraine vs headache distinction is often misunderstood, yet it’s the first crucial step toward finding effective relief and reclaiming your daily life. Many people dismiss their symptoms, but knowing the difference is essential for proper management. This article will clearly break down the key signs, moving beyond the pain itself to reveal the distinct patterns, associated symptoms like nausea or light sensitivity, and even the unique phases that separate a common tension headache from a complex neurological event.
- “It’s not just a headache”: why the difference matters
- The anatomy of pain: a head-to-head comparison
- Beyond the pain: the four phases of a migraine attack
- What about other types of headaches?
- Common triggers: what sets off a migraine vs. a headache?
- When to stop guessing and see a doctor
- References
“It’s not just a headache”: why the difference matters
That throbbing pain behind your eye? The one that makes you want to curl up in a dark room? It’s probably not “just a headache.”
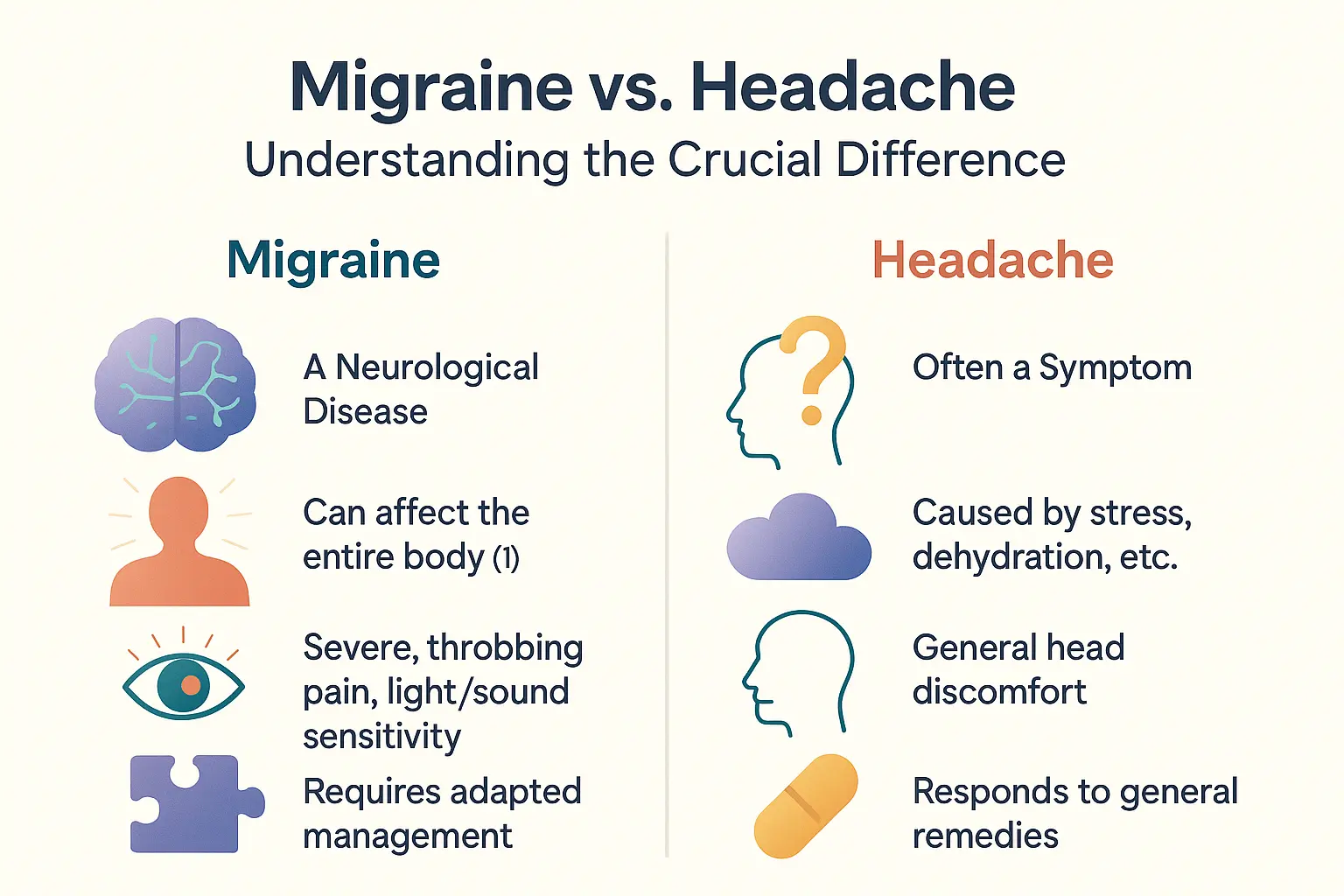
Confusing the two is a common mistake. But it’s an error with real consequences. Many people dismiss intense head pain, but here’s the critical distinction you need to understand: headache is a symptom, often of things like stress or dehydration. A migraine is something else entirely.
In fact, scientific consensus now defines migraine as a complex neurological condition that can affect the entire body. It’s a disease of the nervous system. Not just a bad headache.
Why does this matter so much? Because knowing the difference is the absolute first step toward finding the right kind of relief and getting your life back on track. This isn’t about semantics; it’s about getting the correct help.
So, let’s break down the key signs, without the confusing jargon, to help you finally see clearly what’s going on inside your head.
The anatomy of pain: a head-to-head comparison
Listen to your pain. It’s telling you a story. The way it feels, where it is, what comes with it—these are the first clues to figuring out what’s really going on inside your head. It’s not just “a headache.”
Migraine pain has a distinct personality. Think of it as pulsatile, throbbing, or pounding. A relentless beat. It often picks a side, setting up camp on the left or right of your head—what doctors call a unilateral attack. And forget about trying to “walk it off.” Even the slightest physical activity can make the pain explode.
Then you have the tension headache, which is one of the most common types of headache. This one feels completely different. It’s a dull, constant pressure. Many people describe it as a tight band squeezing their skull. Unlike a migraine, it usually plays fair, affecting both sides of the head at once.
But the differences don’t stop there. A migraine is a full-blown neurological event, bringing along a whole crew of unpleasant symptoms that are almost always absent in a simple tension headache.
| Feature | Migraine | Tension Headache |
|---|---|---|
| Pain Quality | Pulsating, throbbing | Dull, constant pressure (like a band) |
| Pain Location | Often one-sided (unilateral) | Usually both sides (bilateral) |
| Pain Intensity | Moderate to severe, disabling | Mild to moderate, annoying but not disabling |
| Effect of Activity | Pain worsens with physical activity | Pain is not typically worsened by routine activity |
| Associated Symptoms | Nausea, vomiting, extreme sensitivity to light, sound, or smells | Usually none; mild sensitivity to light or sound possible but rare |
| Duration | 4 to 72 hours | 30 minutes to several days |
As you can see, a migraine is a full-body event, not just a pain in the head. The World Health Organization notes that these episodes typically last from 4 to 72 hours, making them a truly disruptive force in one’s life.
Beyond the pain: the four phases of a migraine attack
The biggest thing that sets a migraine apart from a regular headache isn’t just the pain. It’s the fact that a migraine is a process. A journey, really. A standard headache starts and it ends. Simple. But a migraine unfolds in distinct stages—a beginning, a middle, and an end, each with its own character.
Think of it as a neurological event with four distinct phases. Now, not everyone experiences all of them, and they don’t necessarily show up with every single attack. It’s a very personal experience. But understanding them is key.
Here’s how it generally breaks down:
- 1. Prodrome (The “Warning” Phase): This can start up to 24 hours before the headache itself. You might just feel ‘off’—experiencing mood swings, odd food cravings, deep fatigue, or even frequent yawning. It’s your brain’s early warning signal that something is brewing.
- 2. Aura (The “Sensory” Phase): Experienced by about a third of people with migraine, this isn’t just a headache precursor; it’s a full-on neurological event. It can involve visual disturbances like flashing lights or blind spots, tingling sensations, or even difficulty speaking. It typically builds up and can last up to 60 minutes. Understanding the different types of migraine with aura can be incredibly insightful.
- 3. Attack (The “Headache” Phase): This is the main event. The part everyone knows. You get the intense, throbbing pain, often coupled with nausea and extreme sensitivity to light and sound. This is the phase that most people mistakenly call ‘a migraine’.
- 4. Postdrome (The “Hangover” Phase): After the storm passes. The intense pain might be gone, but you can feel completely drained, exhausted, and mentally foggy for a day or two. Many people describe it perfectly as a ‘migraine hangover‘.
This whole sequence, from the first subtle warning to the final exhaustion, demonstrates that a migraine is a complex neurological event. It’s a world away from a simple headache. Recognizing the different phases of a migraine is the first step toward better managing them.
What about other types of headaches?
So, you’ve ruled out a tension headache. But what if your pain doesn’t quite fit the migraine profile either? It’s a common trap to think every bad headache is a migraine. The world of head pain is unfortunately more varied. It’s useful to understand a few other culprits before you talk to a doctor, just so you have the right words to describe what’s happening. You can learn more about other types of headaches to get a fuller picture.
Let’s clear up some frequent mix-ups.
- Sinus headaches: These are the great impostors. They’re often confused with migraine because they cause facial pain. The key differentiator? They are usually accompanied by other sinus infection symptoms, like a thick, discolored nasal discharge and fever. Migraine-related congestion usually involves clear discharge.
- Cluster headaches: These are rare but excruciating. The pain is extremely intense, sharp, and piercing, typically located around one eye. They come on suddenly, in ‘clusters’ or cycles, and are often associated with a droopy eyelid or a stuffy nose on the same side.
If your head pain doesn’t neatly match the description of a migraine or a classic tension headache, don’t dismiss it. Knowing these other possibilities can make your conversation with a healthcare professional much more productive. It helps them pinpoint the real issue faster.
Common triggers: what sets off a migraine vs. a headache?
Understanding what kicks off your head pain is a massive step toward managing it. But not all triggers are equal. The causes of a tension headache are often straightforward. Think stress, exhaustion, or that nagging “tech neck” from poor posture. Simple cause, direct effect.
Migraines are a different beast. The triggers are far more personal and complex. They often stack up until you hit your unique “tipping point.” It’s less about a single cause and more about a perfect storm of factors, making the experience deeply individual.
Here are some of the most frequently reported culprits for migraines.
- Hormonal changes: Many women experience migraines linked to their menstrual cycle, a classic and frustrating pattern.
- Specific foods and drinks: The list of potential migraine food triggers includes aged cheeses, processed meats, alcohol (especially red wine), and caffeine—both too much and withdrawal from it.
- Sensory stimuli: Bright lights, loud noises, and strong smells like perfume can feel like a direct assault and act as potent triggers.
- Changes in routine: This is a big one. The migraine brain craves consistency. Skipping a meal, irregular sleep, or a shift in the weather can set off an attack.
These are just some of the common migraine triggers. Your most powerful tool is knowledge. Consider keeping a journal. Tracking your days—what you ate, how you slept, your stress levels—helps you connect the dots and identify personal trigger patterns. It’s a game-changer.
When to stop guessing and see a doctor
Self-diagnosis is a starting point, not a destination. While it’s tempting to Google your symptoms, that path has its limits and can create unnecessary anxiety.
Consider seeing a doctor if your headaches—any kind—are frequent, severe, or if they start to disrupt your daily life. When a headache interferes with your work or family, it’s a clear signal you need professional guidance.
Then there are the “red flags.” These aren’t suggestions; they are urgent calls for immediate medical attention. Pay close attention to these signs highlighted by sources like Harvard Health:
- A sudden, severe headache like a “thunderclap,” peaking in under a minute.
- Headache with fever, a stiff neck, confusion, seizures, or a rash.
- A headache that develops after a head injury.
- A new type of headache, especially if you’re over 50.
- A headache that worsens despite treatment.
Most headaches aren’t dangerous. But getting a correct diagnosis is the absolute key to managing the pain and taking back control of your life.
References
To ensure the information provided is accurate and trustworthy, this article relies on established medical classifications and health organizations. Here are the primary sources used for our explanations.
- International Headache Society (IHS): The International Classification of Headache Disorders, 3rd edition (ICHD-3), is the global standard for diagnosing and classifying headache disorders.
- World Health Organization (WHO): Provides global public health guidance and data on the prevalence and impact of headache disorders, including migraine.
Understanding the difference between a migraine and a headache is more than just semantics; it’s the first step toward effective management. A migraine is a complex neurological event, not just a bad headache. By recognizing your specific symptoms, identifying triggers, and knowing when to seek help, you can move beyond guessing and start your journey toward regaining control.