For the 12-60% of migraine sufferers sensitive to food triggers, what you eat isn’t the root cause but a catalyst. Scientific Reports 2024 shows tyramine, nitrates, or histamine can activate attacks in predisposed individuals. Tracking personal patterns via a food diary beats generic lists, avoiding unnecessary restrictions. Remember: consistency in meals and hydration matters more than chasing mythical “bad foods.”
Ever wondered why your morning coffee or favorite cheese might be silently fueling your migraines? While migraine food triggers vary widely—from aged cheeses and processed meats to alcohol and artificial sweeteners—understanding their role can feel like solving a puzzle. Did you know studies suggest only 10-60% of migraineurs report diet-related triggers? This article breaks down the science, separates myths from facts (like caffeine’s dual role), and offers actionable strategies—from tracking hidden additives to prioritizing hydration and stable blood sugar. Discover how personalized habits, not strict bans, could reduce your risk without sacrificing joy.
- Understanding the link between food and migraine
- Food Craving: A Trigger Or A Migraine Warning Sign?
- How to identify your personal food triggers
- General dietary habits for migraine prevention
- A personalized approach is key to managing your diet
Understanding the link between food and migraine
What is a food trigger for migraine?
Food triggers are specific items that may precipitate a migraine attack in predisposed individuals, but they are not the root cause of the disease itself. Think of it like a light switch: the wiring (genetic and neurological factors) exists first, and the switch (food) simply activates it.
According to a 2024 study in Scientific Reports, only 12–60% of migraine patients report food as a trigger. This wide range shows how individualized these responses are. Unlike allergies or intolerances, triggers work through complex neurological pathways rather than immune reactions.
Why triggers are highly personal and complex
There is no universal “avoid” list for migraineurs. A food that sparks a crisis in one person might be perfectly safe for another. This variability stems from:
- Threshold theory: A single trigger might not matter alone, but multiple factors (like stress + skipped meal + certain food) can push someone over their personal “migraine threshold”
- Delayed reactions: Symptoms might appear up to 24 hours after consumption, making patterns hard to spot without tracking
Research in Headache (2019) confirms scientific evidence remains inconsistent for most foods. For deeper context, understanding other migraine causes and triggers helps build a complete picture of this multifactorial condition.
Migraine is a neurological disease with genetic roots. Food triggers act as environmental modifiers that interact with this biological terrain. While associations exist between migraines and items like aged cheeses, alcohol, or processed meats, these links don’t prove causation. The key takeaway? Track your responses individually and prioritize regular meals over blanket dietary restrictions.
| Food/Drink Category | Potential Triggering Substance | Common Examples | Important Notes |
|---|---|---|---|
| Aged Cheeses | Tyramine | Cheddar, Brie, Blue cheese | Tyramine forms as proteins break down in aging foods. Migraine Quebec notes these cheeses are frequent triggers. Cadaverine and other amines may amplify effects through synergistic reactions. |
| Processed & Cured Meats | Nitrites/Nitrates | Hot dogs, Bacon, Salami | Preservatives linked to American Migraine Foundation research showing oral Streptococcus bacteria convert nitrates to migraine-inducing compounds. Cold cuts with “no added nitrates” may still contain natural sources from celery juice. |
| Alcohol | Histamine, Sulfites, Dehydration | Red wine, Beer | Alcohol causes dehydration – a known trigger. Red wine contains both histamine and tyramine, Migraine Buddy tracks this as top reported trigger. Carbonated options like champagne accelerate alcohol absorption. |
| Chocolate | Phenylethylamine | Milk chocolate, Dark chocolate | Controversial trigger – Voix des Migraineux highlights conflicting studies. Some evidence suggests chocolate cravings may be premonitory symptoms rather than cause, with 12% of sufferers misattributing attacks to consumption. |
| Fermented Foods | Tyramine, Histamine | Sauerkraut, Soy sauce, Kimchi | Traditional preservation methods increase amine content. Migraine.fr reports 10-15% of sufferers identify this trigger. Kombucha contains multiple amines and alcohol byproducts that may compound effects. |
| Foods with MSG | Monosodium Glutamate | Some soy sauces, Processed foods | Common additive in Asian cuisine. Japanese research links high-dose exposure to glutamate receptor activation, though typical dietary amounts rarely reach problematic levels for most individuals. |
| Artificial Sweeteners | Aspartame | Diet sodas, Sugar-free gum | Linked to headaches in 8.2% of migraineurs according to clinical studies. Effects often delayed by 24-48 hours, making identification challenging without tracking. |
| Certain Fruits & Vegetables | Tyramine, Histamine | Ripe bananas, Citrus, Avocados, Onions | Natural compounds increase with ripeness. Tomatoes contain tyramine and histamine in varying concentrations. Migraine Quebec specifically warns about overripe produce and aged garlic pastes. |
The Special Case of Caffeine: Friend or Foe?
Caffeine presents a paradoxical relationship with migraines. For some sufferers, small amounts (50-100mg) can effectively treat attacks by constricting blood vessels and enhancing pain medication absorption. However, regular consumption exceeding 200mg/day creates physical dependence.
This dependency creates a dangerous cycle: sudden cessation causes withdrawal headaches in 70% of overusers. The American Migraine Foundation emphasizes maintaining consistent intake patterns to avoid fluctuations. For context, a standard coffee contains 80-100mg caffeine, while energy drinks can pack 200mg+ per can. Even decaf coffee contains 3-17mg per cup that may accumulate.
- Limited to 1-2 servings daily of standard strength coffee or tea
- Avoid abrupt changes to consumption patterns, including weekend binges
- Choose naturally caffeinated sources over synthetic versions in energy shots
- Monitor individual tolerance through headache diaries for 4-6 weeks minimum
Crucially, caffeine’s effects vary dramatically. While some find it helpful during attacks, others experience immediate triggering – highlighting the importance of personal tracking over generalized avoidance. Migraine Buddy data shows gradual reduction works better than abrupt elimination for long-term management.
Food Craving: A Trigger Or A Migraine Warning Sign?
Understanding The Migraine Prodrome Phase
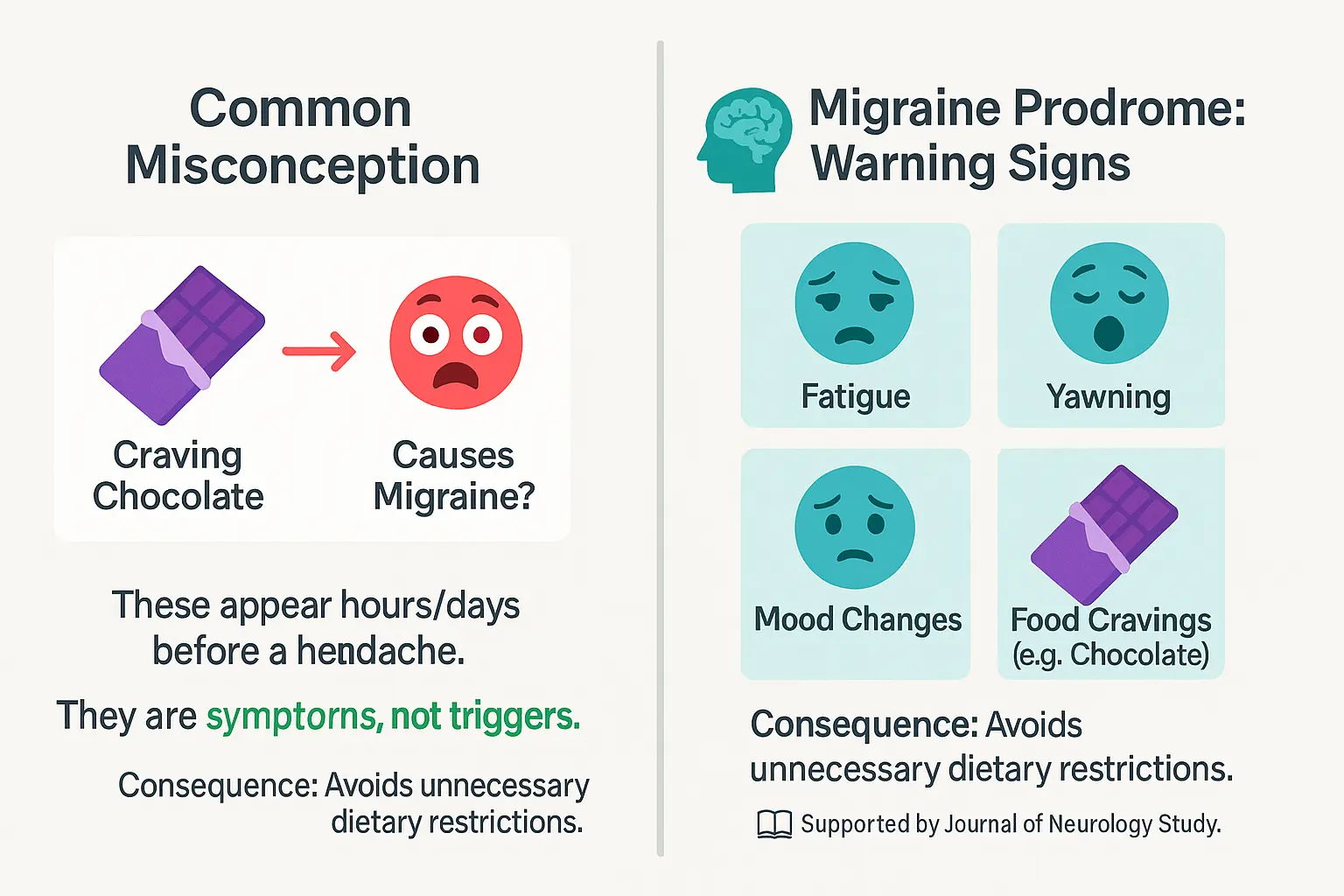
Migraine attacks often begin with a prodrome phase, occurring hours or even days before head pain. This early stage includes subtle symptoms like fatigue, mood shifts, excessive yawning, and food cravings — often mistaken for triggers.
Cravings for chocolate, salty snacks, or other specific foods may not cause migraines but instead signal that a neurological cascade has already started. Recognizing these signs helps patients act early, potentially reducing attack severity. For example, taking acute medication during this phase can prevent full-blown pain.
Understanding all migraine phases prevents misattributing symptoms to external factors like diet. Common prodrome signs include neck stiffness, light sensitivity, and altered appetite. These cues offer a critical window for intervention.
The Chocolate Example: Misinterpreting The Signs
Chocolate is frequently blamed for migraines. However, research in the Journal of Neurology reveals cravings often reflect prodromal brain changes, not causation. People eat chocolate as their brain already initiates a migraine, then wrongly link it to the attack.
This confusion leads to unnecessary food restrictions. Only 10% of migraineurs have confirmed dietary triggers, yet many eliminate entire food groups. For most, chocolate’s magnesium and riboflavin content — both migraine-preventive nutrients — makes it safe when consumed in moderation.
Tracking symptoms in a migraine journal clarifies true triggers. If headaches consistently follow chocolate by 24 hours, consider elimination. Otherwise, avoid self-imposed dietary limits that may worsen quality of life. Always consult healthcare providers for personalized strategies.
- Key takeaway: Food cravings may signal prodrome, not causation
- Action step: Use journals to distinguish symptoms from triggers
- Prevention tip: Stay hydrated and eat regular meals to avoid low blood sugar
How to identify your personal food triggers
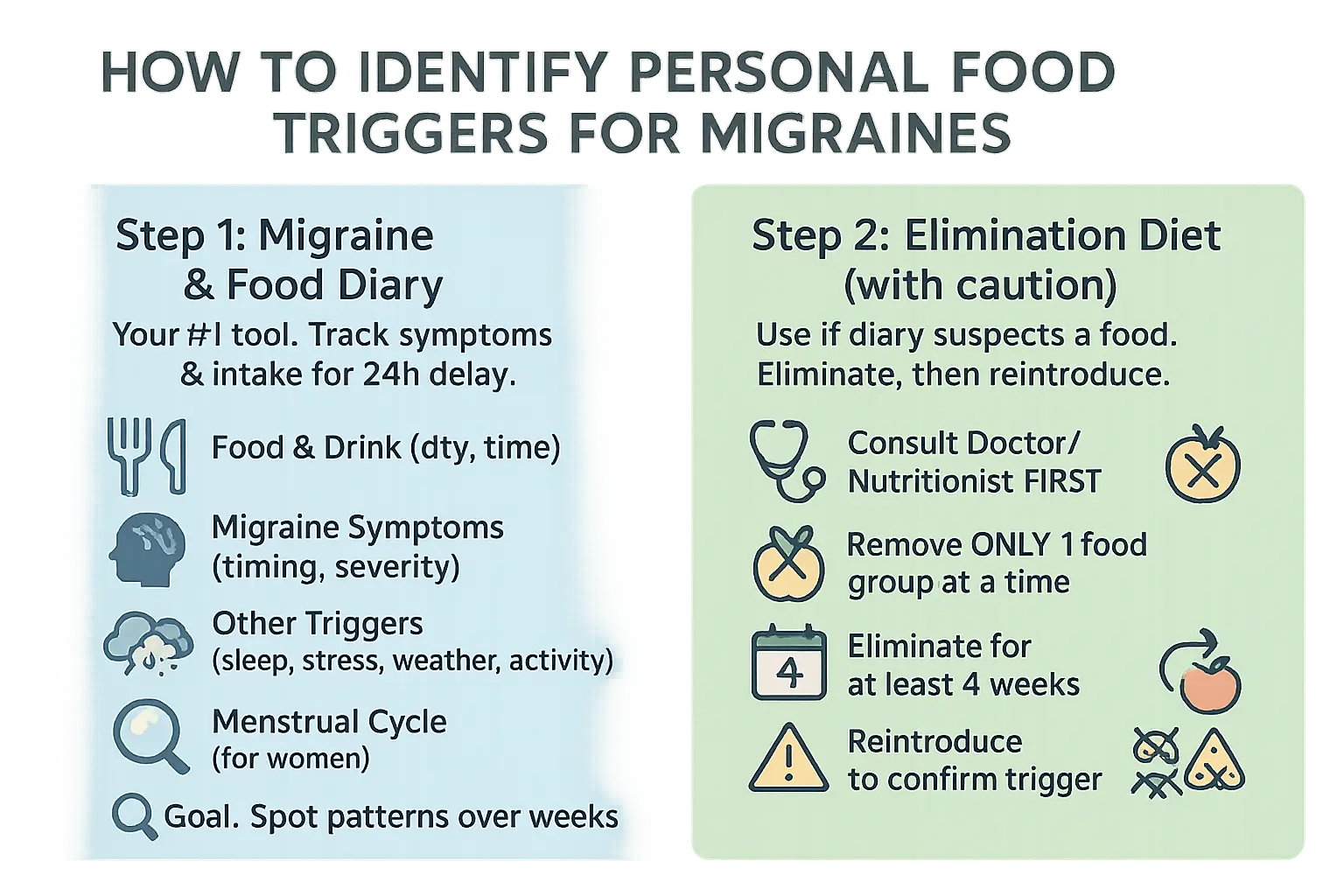
Keeping a detailed migraine and food diary
Tracking your diet is the most reliable way to identify personal migraine triggers. Symptoms can appear up to 24 hours after eating, making a detailed journal essential. According to Harvard Health, this method allows you to spot patterns that might otherwise go unnoticed.
What to track in your migraine diary:
- Everything you eat and drink, including quantities and time of day
- The timing and severity of any migraine symptoms you experience
- Other potential triggers: sleep duration and quality, stress levels, weather changes, physical activity
- For women, the timing of your menstrual cycle
This systematic approach helps distinguish between true food triggers and coincidence. Many migraine patients wrongly blame chocolate or cheese without realizing these might simply be cravings during pre-migraine phases. The diary reveals actual cause-effect relationships over weeks, not just isolated incidents. For example, you might notice migraines often follow days with skipped meals or dehydration, even if you avoid commonly reported triggers like aged cheeses.
Using an elimination diet (with caution)
When your journal points to a specific food, an elimination diet can confirm suspicions. This method requires careful implementation to avoid nutritional deficiencies while getting clear results. Always work with a healthcare professional to ensure safe execution. For instance, if sulfite-containing dried fruits or aspartame-sweetened drinks consistently appear before attacks, removing them for 4 weeks reveals whether symptoms improve.
Key principles of an elimination diet:
- Consult a doctor or nutritionist before starting
- Remove only one suspected food group at a time to avoid nutritional deficiencies and get clear results
- Keep the elimination period for at least 4 weeks
- If you feel better, reintroduce the food to confirm it’s a trigger
- Never eliminate too many food groups at once
This method helps test specific suspects identified through your journal. For example, tyramine in aged cheeses or monosodium glutamate (MSG) in processed snacks often emerge as culprits. The reintroduction phase is critical: consume the food daily for 3-5 days while monitoring symptoms, as delayed reactions can occur. Individual responses vary—what affects one person won’t necessarily impact others. Remember, the goal isn’t permanent restriction but understanding your unique sensitivities while maintaining nutritional balance and hydration. Tools like the Migraine Buddy app can simplify tracking progress during elimination phases.
General dietary habits for migraine prevention
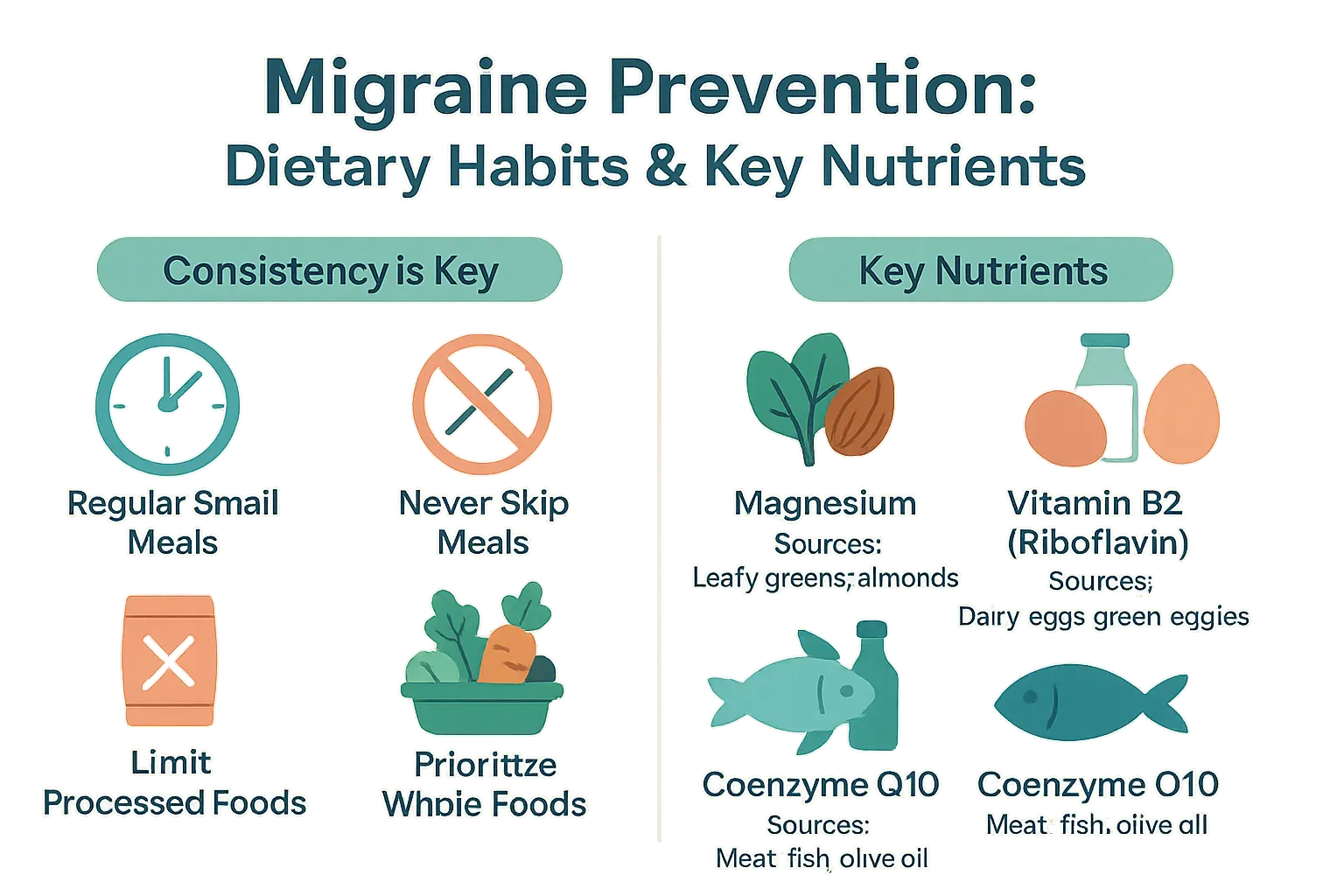
The importance of consistency: meals and hydration
Migraine brains thrive on predictable patterns. Sudden changes in glucose availability can destabilize brain energy metabolism, creating conditions for attacks. Research shows that intermittent fasting or prolonged meal gaps trigger migraines in 30-50% of patients by causing blood sugar drops that activate stress hormone release. Dehydration exacerbates this effect, with studies confirming that 84% of migraineurs experience dehydration as a direct trigger.
- Foundational habits for migraine prevention:
- Consume small, balanced meals every 3-4 hours to maintain stable blood sugar levels and prevent neuroinflammation.
- Make breakfast non-negotiable – skipping it increases risk by 12% according to population studies.
- Hydrate proactively with 8-10 cups water daily, prioritizing plain water over flavored/sugary drinks that might contain hidden triggers.
- Replace ultra-processed options with whole foods to reduce exposure to artificial additives and support gut-brain axis health.
- Build meals around protein and complex carbohydrates to slow glucose absorption and maintain satiety between meals.
These practices work synergistically with other lifestyle modifications in comprehensive migraine management, emphasizing consistency rather than perfection.
Nutrients that may play a supportive role
Clinical research identifies specific micronutrients with migraine-modulating properties. While dietary sources remain preferable, supplementation shows promise when monitored:
- Magnesium – Found in spinach, quinoa, and pumpkin seeds, this “anti-stress mineral” regulates calcium channels and reduces cortical spreading depression. Double-blind trials show 400-600mg daily prevents attacks by improving mitochondrial efficiency.
- Vitamin B2 (Riboflavin) – Crucial for ATP production in brain cell mitochondria. Studies reveal 400mg/day reduces both frequency and acute medication use, with benefits becoming apparent after 8-12 weeks.
- Coenzyme Q10 – Acts as both antioxidant and mitochondrial booster. Randomized controlled trials demonstrate 300mg daily decreases inflammatory markers like CGRP while enhancing cellular energy production.
Supplementation requires professional oversight due to potential interactions with medications. For example, magnesium may interfere with bisphosphonates, while CoQ10 can affect blood thinner efficacy. Always consult your neurologist before adding supplements to your regimen.
A personalized approach is key to managing your diet
Studies suggest that only 10% of migraine sufferers have food-related triggers, yet identifying them is highly individual. What sparks a crisis for one may be safe for another.
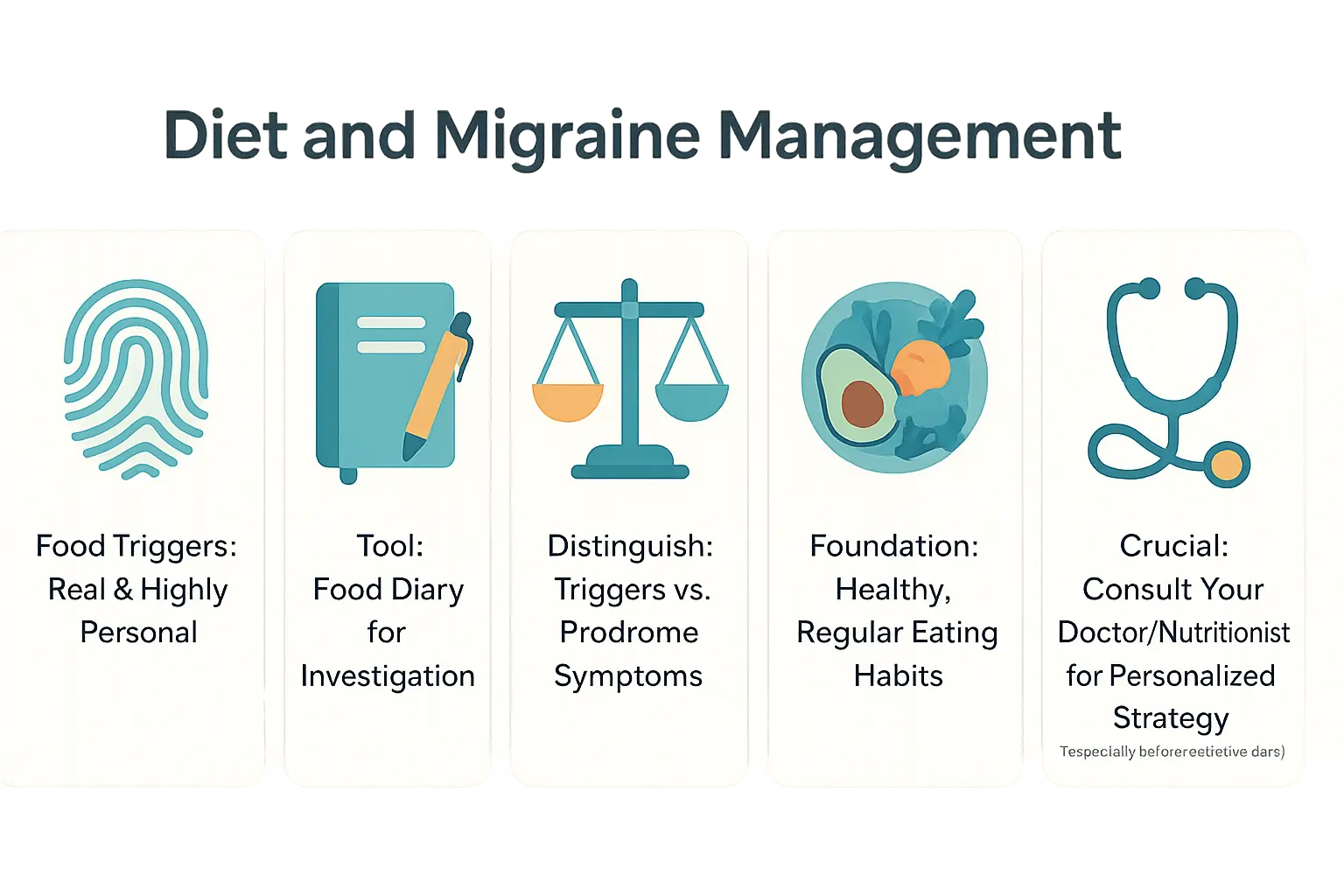
Your path forward with food and migraines
Food triggers exist but vary widely. Research links migraines to aged cheeses, alcohol, and processed meats, but your biology decides your sensitivities. A food diary helps distinguish real triggers from coincidences by tracking meals and symptoms.
Chocolate cravings often signal the prodrome phase—the brain’s early warning system. Experts clarify that these cravings are symptoms, not causes, of migraines.
Skipping meals or fasting drops blood sugar, a trigger for some. Data shows 75–90% experience prodrome symptoms like fatigue or cravings up to 24 hours pre-migraine. Staying hydrated and eating balanced meals stabilizes this risk.
Eliminating foods without guidance risks nutritional gaps. Migraine France warns restrictive diets may raise stress—a paradoxical trigger. Work with a doctor to test suspected foods systematically, removing one at a time for four weeks.
This article is informational, not medical advice. Migraines are complex; no single diet fits all. Consult a physician or nutritionist for strategies balancing caution and enjoyment, avoiding unnecessary restrictions.
In managing migraines, understanding your unique triggers is crucial. While foods aren’t universal causes, tracking meals and symptoms in a diary can reveal patterns. Stay hydrated, eat regularly, and consult a healthcare provider before major dietary changes. Personalized strategies, not strict bans, offer the best path forward.
FAQ
What’s the most common food linked to migraine attacks?
While triggers vary from person to person, research suggests that alcohol—especially red wine—is one of the most frequently reported food triggers. A 2024 study in Scientific Reports found that around 20-30% of migraine sufferers identify alcohol as a trigger. However, it’s important to understand that what causes a migraine in one person might not affect another. Other common triggers include aged cheeses, processed meats, and foods containing MSG. The key is to listen to your body and track your personal patterns.
What are the key dietary habits to prevent migraines?
Think of the “5 Cs” as a simple framework for migraine-friendly eating:
- Consistency: Eat regular meals to maintain stable blood sugar
- Choices: Opt for fresh, whole foods over processed options
- Chocolate: Enjoy in moderation, as it can be both a comfort and a potential trigger
- Caffeine: Use cautiously – small amounts might help, but excess can backfire
- Connection: Track your food and symptoms to understand your personal patterns
These habits help create a stable environment for your brain, which is especially important for migraine sufferers.
Which foods are most likely to trigger migraines?
Common culprits include:
- Aged cheeses (cheddar, blue cheese) with tyramine
- Processed meats (hot dogs, bacon) containing nitrates
- Alcohol (especially red wine) causing dehydration
- Chocolate with phenylethylamine
- Fermented foods (kimchi, soy sauce) with histamine
- Products with MSG (some processed foods)
- Artificial sweeteners like aspartame
- Very ripe bananas with tyramine
Remember, these foods don’t cause migraines for everyone. A 2019 systematic review in Headache noted that only about 12-60% of migraine sufferers report food triggers. The best approach is personal tracking through a food diary.
Can migraines cause nausea and vomiting?
Yes, nausea and vomiting are common symptoms during a migraine attack, affecting about 90% of people with migraines according to the American Migraine Foundation. These symptoms often develop alongside the headache phase and can be caused by the same neurological processes that cause pain. The gut-brain connection means migraines can slow digestion, leading to nausea. If you experience severe vomiting, discuss management options with your doctor.
Is there a permanent cure for migraines?
Currently, there’s no permanent cure for migraines, but effective management strategies exist. Think of migraines like chronic conditions such as asthma – while not curable, they can be controlled. Treatment approaches include acute medications (like triptans), preventive medications (beta-blockers, CGRP inhibitors), lifestyle modifications, and alternative therapies. The goal is reducing frequency and severity to improve quality of life through personalized management plans with your neurologist.
What should you eat during a migraine attack?
During an attack, try these options:
- Ginger tea to help with nausea
- Hydration with water or electrolyte drinks
- Plain carbohydrates like toast (easy to digest)
- Small portions of bland foods if hungry
- Room temperature foods if smells bother you
Avoid strong smells, spicy foods, and anything that seems to worsen your symptoms. Remember, food won’t stop a migraine once it starts, but good nutrition supports overall brain health and recovery.
Which vitamins help prevent migraines?
Research shows several vitamins can help:
- Riboflavin (B2): 400 mg/day can reduce frequency (found in dairy, eggs)
- Magnesium: 400-600 mg/day (found in leafy greens, nuts)
- CoQ10: 100 mg three times daily (found in fish, meats)
A 2020 study in the Journal of Neurology showed these supplements can reduce migraine frequency by 50% in some patients. Always consult your doctor before starting supplements, as they can interact with medications.
What causes migraines?
Migraines result from complex brain activity involving:
- Genetic predisposition (family history plays a role)
- Neurochemical changes (serotonin fluctuations)
- Trigeminal nerve activation (pain pathway)
- Genetic mutations affecting ion channels
It’s like having a sensitive “alarm system” in your brain. When various factors (triggers) combine, they activate this system, causing the pain and symptoms. While we don’t know the exact “root” cause, we understand the mechanisms well enough to develop effective treatments.
Are bananas a migraine trigger?
Some people report bananas as a trigger due to tyramine, especially very ripe ones. However, bananas are also rich in potassium, magnesium, and B6 – nutrients that support brain health. A 2020 study found what people perceive as triggers might actually be early symptoms. The banana craving could be your brain signaling an attack before pain starts. If you suspect bananas, track them in your diary before eliminating them from your diet.